What is generalized osteoarthritis? This condition affects multiple joints, unlike localized forms of arthritis. Understanding its characteristics, causes, diagnosis, and treatment is crucial for those affected. We’ll explore the various facets of this complex ailment, from its defining features to the potential long-term implications.
Generalized osteoarthritis, a multifaceted condition, encompasses a range of symptoms and challenges. This comprehensive guide provides a thorough understanding of the different types, stages, and treatments for generalized osteoarthritis, along with an insightful look at risk factors and preventative measures.
Defining Generalized Osteoarthritis
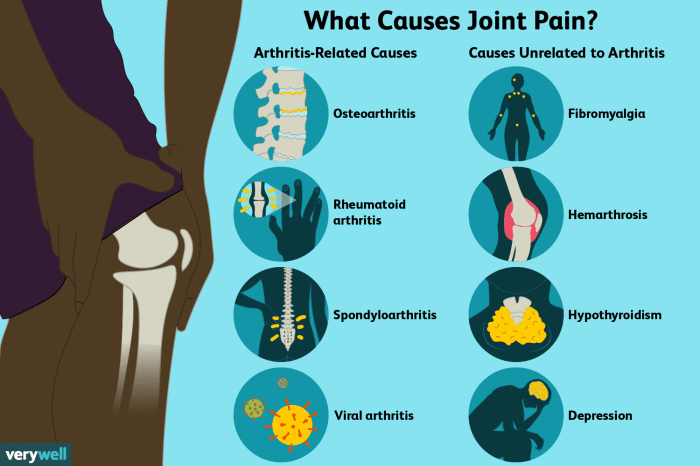
Generalized osteoarthritis, unlike localized forms, affects multiple joints simultaneously. This condition presents a unique challenge due to the widespread nature of the joint pain and stiffness. Understanding its characteristics and distinguishing it from other types of arthritis is crucial for proper diagnosis and management. The impact on daily life can be substantial, requiring careful consideration of treatment options and lifestyle modifications.
Defining Generalized Osteoarthritis
Generalized osteoarthritis encompasses a spectrum of conditions characterized by the progressive breakdown and degeneration of cartilage within multiple joints. This contrasts with localized osteoarthritis, which typically affects one or a few specific joints. The underlying causes can vary, but they often involve a combination of genetic predisposition, mechanical stress on joints, and the aging process.
Key Characteristics
Generalized osteoarthritis distinguishes itself from other forms of arthritis through several key features. The simultaneous involvement of multiple joints is a primary characteristic. Symptoms tend to be symmetrical, meaning they appear on corresponding joints on both sides of the body. This symmetry helps clinicians differentiate it from conditions that affect joints unevenly. Furthermore, the progressive nature of the condition is evident, with symptoms typically worsening over time.
This slow, chronic deterioration contrasts with the potentially more acute onset of some other forms of arthritis.
Types of Generalized Osteoarthritis
While the term “generalized osteoarthritis” itself doesn’t precisely delineate specific types, certain underlying conditions can contribute to a generalized pattern of joint involvement. Examples include conditions like inflammatory arthritis, where systemic inflammation can lead to joint damage. In these cases, the osteoarthritis is often a secondary consequence of the underlying inflammatory process.
Common Symptoms
The symptoms of generalized osteoarthritis are typically chronic and gradually progressive. Common complaints include persistent joint pain, stiffness, and reduced range of motion. Pain is often worse after periods of inactivity or prolonged use of the affected joints. Morning stiffness, lasting for 30 minutes or more, is also a frequent symptom. Tenderness to the touch over affected joints is also a frequent characteristic.
Generalized osteoarthritis is a condition where the cartilage in your joints wears down over time, leading to pain and stiffness. While the exact causes of this wear and tear are complex, lifestyle choices and underlying health issues like those often linked to what causes low testosterone in young males can play a role. Ultimately, osteoarthritis is a progressive condition, impacting mobility and daily life.
Understanding its potential causes is key to managing it effectively.
Joint swelling and creaking sounds within the joint can occur as the disease progresses.
Stages of Generalized Osteoarthritis
| Stage | Description | Joint Involvement | Symptoms |
|---|---|---|---|
| Early Stage | Cartilage damage begins. | Limited joint involvement. | Mild pain, stiffness, and reduced range of motion, particularly after periods of inactivity. |
| Moderate Stage | Significant cartilage loss. | More joints involved, often symmetrically. | Increased pain, stiffness, and limitations in daily activities. Morning stiffness may last longer. |
| Severe Stage | Extensive cartilage loss and bone changes. | Majority of joints are affected. | Severe pain, significant loss of joint function, and considerable limitations in daily activities. |
Note: The stages above are generalized representations. Individual experiences and disease progression can vary significantly. Medical consultation is crucial for accurate assessment and tailored management strategies.
Causes and Risk Factors: What Is Generalized Osteoarthritis
Understanding the causes and risk factors of generalized osteoarthritis is crucial for prevention and management. While the exact mechanisms behind this condition remain somewhat elusive, researchers have identified several potential contributing factors, ranging from genetics to lifestyle choices. This exploration delves into the complexities of generalized osteoarthritis, examining the interplay of these factors to provide a more comprehensive understanding of this prevalent condition.
Generalized osteoarthritis is a common condition where cartilage in joints wears down, causing pain and stiffness. While the exact causes are complex, it’s often linked to factors like aging and genetics. Sometimes, other inflammatory conditions like, for example, terminal ileitis overview and more , can indirectly impact joint health, though the relationship isn’t always clear. Ultimately, understanding the various factors that contribute to generalized osteoarthritis is key to managing the condition effectively.
Potential Causes
Generalized osteoarthritis isn’t a single, easily identifiable cause. Instead, a complex interplay of factors contributes to its development. Researchers believe that a combination of genetic predisposition, environmental influences, and lifestyle choices play critical roles. For instance, some individuals may inherit a tendency towards joint degradation, while others may develop the condition due to repetitive stress or obesity.
This complex interplay is a key aspect of the condition’s etiology.
Risk Factors
Numerous factors increase an individual’s susceptibility to generalized osteoarthritis. Understanding these risk factors can aid in preventative measures and early intervention.
- Age: The risk of osteoarthritis increases significantly with age. Cartilage naturally degrades over time, and this degradation accelerates with advancing years. This progressive decline in cartilage quality often leads to joint pain and stiffness, particularly in older adults.
- Genetics: Genetic predisposition plays a substantial role in the development of osteoarthritis. Certain genes may increase the risk of cartilage breakdown and joint inflammation. Individuals with a family history of osteoarthritis are at higher risk of developing the condition themselves.
- Obesity: Excess weight places significant stress on weight-bearing joints, such as the knees and hips. This constant pressure can accelerate cartilage wear and tear, increasing the likelihood of osteoarthritis. Studies consistently demonstrate a strong correlation between obesity and the development of knee and hip osteoarthritis.
- Repetitive Stress: Jobs or activities that involve repetitive movements or high-impact loading can strain joints, potentially leading to osteoarthritis. Athletes, manual laborers, and those in professions requiring repetitive motions may experience increased risk.
- Joint Injuries: Previous injuries to a joint, such as fractures or ligament tears, can increase the risk of developing osteoarthritis later in life. These injuries often result in abnormal joint mechanics, leading to accelerated cartilage degeneration.
Comparison with Other Forms of Arthritis
While generalized osteoarthritis shares some overlapping risk factors with other forms of arthritis, there are crucial distinctions. For example, rheumatoid arthritis, a chronic autoimmune disease, involves inflammation of the joints, often characterized by symmetrical joint involvement. In contrast, generalized osteoarthritis is primarily characterized by the breakdown of cartilage, with a more gradual onset and less prominent inflammatory component.
Other types of arthritis, such as gout, are associated with different underlying causes and mechanisms, and their risk factors differ accordingly.
Role of Genetics
Genetic factors play a crucial role in the development of generalized osteoarthritis. Specific genes can influence cartilage production, metabolism, and overall joint health. While genes alone don’t guarantee the development of the condition, they create a predisposition or susceptibility to osteoarthritis. Individuals with a family history of osteoarthritis are more likely to develop the condition themselves.
Summary of Risk Factors
| Risk Factor | Category | Description |
|---|---|---|
| Age | Non-modifiable | Risk increases with advancing years due to natural cartilage degradation. |
| Genetics | Non-modifiable | Certain genes can increase susceptibility to cartilage breakdown and joint inflammation. |
| Obesity | Modifiable | Excess weight puts significant stress on weight-bearing joints, accelerating cartilage wear and tear. |
| Repetitive Stress | Modifiable | Jobs or activities involving repetitive movements or high-impact loading can strain joints. |
| Joint Injuries | Modifiable (to some extent) | Previous injuries can lead to abnormal joint mechanics, accelerating cartilage degeneration. |
Diagnosis and Evaluation
Diagnosing generalized osteoarthritis often involves a multifaceted approach, combining patient history, physical examination, and diagnostic imaging. This comprehensive evaluation helps determine the extent of joint involvement and the severity of the condition, ultimately guiding treatment strategies. Careful consideration of various factors, including age, lifestyle, and family history, is crucial for an accurate diagnosis.
Diagnostic Procedures
A thorough patient history plays a pivotal role in the diagnostic process. Information gathered includes the duration and progression of symptoms, specific joint locations affected, associated pain characteristics (e.g., intensity, location, duration), and any relevant medical history. This detailed history helps narrow down potential causes and identify potential risk factors. A comprehensive physical examination follows, focusing on range of motion, tenderness, and the presence of any deformities in affected joints.
The examiner will assess the patient’s ability to perform daily activities and evaluate their overall functional status.
Methods for Evaluating Severity, What is generalized osteoarthritis
Several methods exist for evaluating the severity of generalized osteoarthritis. These include clinical scales and questionnaires designed to assess the impact of the condition on daily life. The Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) is a widely used instrument that evaluates pain, stiffness, and physical function. Other relevant assessments include the Health Assessment Questionnaire (HAQ) and the Arthritis Impact Measurement Scales (AIMS).
These tools provide quantitative measures of the disease’s impact, allowing for tracking progress and evaluating treatment effectiveness.
Physical Examination Tools
The physical examination relies on several tools and techniques to assess joint function and structural changes. Range of motion (ROM) measurements are taken for each affected joint, documenting the extent of movement possible. Palpation (touching) identifies areas of tenderness or swelling. Observation of gait and posture provides insights into the impact of joint pain on movement patterns.
Muscle strength testing is also performed to evaluate the potential involvement of associated muscle groups. This process allows clinicians to quantify the effects of the condition and evaluate the overall impact on the patient’s functional ability.
Diagnostic Imaging Techniques
Several imaging modalities may be used to aid in the diagnosis of generalized osteoarthritis. X-rays are frequently employed to visualize joint spaces, bone density, and the presence of osteophytes (bone spurs). These images can reveal narrowing of the joint space, a hallmark sign of osteoarthritis. Magnetic resonance imaging (MRI) can provide more detailed information about cartilage damage, soft tissue inflammation, and bone marrow lesions.
Computed tomography (CT) scans can assess bone structure in greater detail. These advanced imaging techniques are employed when X-rays alone do not provide sufficient information or when more detailed evaluation of soft tissues is required.
Flowchart of Diagnostic Process
The above flowchart provides a simplified visual representation of the diagnostic process for generalized osteoarthritis. Note that the specific tests and procedures may vary depending on the individual patient’s situation and the presenting symptoms.
Treatment and Management
Generalized osteoarthritis, while a progressive condition, is manageable. Effective treatment strategies often involve a multifaceted approach, encompassing both non-pharmacological interventions and, when necessary, pharmacological therapies. Understanding the available options and tailoring a personalized plan is crucial for maximizing comfort and function.Effective management of generalized osteoarthritis requires a combination of approaches that address pain, stiffness, and functional limitations. A holistic strategy that integrates lifestyle modifications, physical therapies, and, if appropriate, medication can significantly improve quality of life.
Non-Pharmacological Approaches
Non-pharmacological interventions form the cornerstone of initial osteoarthritis management. These strategies aim to reduce pain, improve mobility, and maintain joint function without relying on medication. These methods are often highly effective in conjunction with lifestyle changes and can be particularly beneficial in early stages of the disease.
- Physical Therapy: Physical therapists design individualized exercise programs that target specific muscle groups supporting affected joints. These exercises can improve joint stability, flexibility, and range of motion. Examples include strengthening exercises for the knees, hip stretches, and low-impact aerobic activities. Proper technique and consistent adherence to the therapy plan are essential for positive outcomes.
- Assistive Devices: Assistive devices, such as canes, walkers, and braces, can help reduce stress on affected joints. Proper selection and use of these devices can improve mobility and reduce pain. Consideration should be given to factors like joint involvement, patient’s physical abilities, and desired level of independence.
- Occupational Therapy: Occupational therapists assess and modify the patient’s home and work environments to improve functionality and reduce strain on affected joints. This might include adapting household tasks, modifying workspaces, and recommending ergonomic strategies. The goal is to create an environment that supports the patient’s daily activities and minimizes the risk of further joint damage.
- Heat and Cold Therapy: Applying heat or cold packs to affected joints can help alleviate pain and stiffness. Heat promotes blood flow, which can reduce muscle tension and pain. Cold therapy can help reduce inflammation and swelling. These methods are often used in conjunction with other therapies.
Lifestyle Modifications
Lifestyle modifications play a significant role in managing generalized osteoarthritis. Adopting healthy habits can reduce the burden of the condition and improve overall well-being.
- Weight Management: Maintaining a healthy weight is crucial. Excess weight puts added stress on weight-bearing joints, accelerating cartilage breakdown and pain. A balanced diet and regular exercise are essential components of a weight management plan.
- Regular Exercise: Regular low-impact exercise, such as swimming, cycling, or walking, can strengthen muscles around joints, improve flexibility, and maintain joint mobility. A personalized exercise routine, tailored to individual needs and abilities, is important for safe and effective results.
- Proper Posture and Body Mechanics: Maintaining good posture and using proper body mechanics during daily activities can reduce stress on affected joints. This includes avoiding prolonged periods of standing or sitting, and using appropriate lifting techniques.
Pharmacological Treatment
Medication plays a supporting role in managing generalized osteoarthritis symptoms. Pain relievers and other medications are prescribed to alleviate pain and inflammation. However, it’s crucial to consult a physician to determine the appropriate medication and dosage.
- Analgesics (Pain Relievers): Over-the-counter pain relievers, such as ibuprofen or acetaminophen, can help manage mild to moderate pain. Prescription-strength analgesics may be necessary for more severe pain. It’s important to follow dosage instructions carefully and consult a doctor if side effects occur.
- Disease-Modifying Anti-Rheumatic Drugs (DMARDs): In some cases, DMARDs may be prescribed to slow the progression of osteoarthritis. These medications are typically reserved for individuals with more severe disease.
Treatment Options Table
| Treatment Category | Treatment Options |
|---|---|
| Non-Pharmacological | Physical Therapy, Assistive Devices, Occupational Therapy, Heat/Cold Therapy |
| Pharmacological | Analgesics (Over-the-counter/Prescription), Disease-Modifying Anti-Rheumatic Drugs (DMARDs) |
Prognosis and Complications
Generalized osteoarthritis, while not always debilitating, can significantly impact a person’s quality of life. Understanding the potential long-term effects and associated complications is crucial for effective management and proactive strategies. A proactive approach allows individuals to address potential issues early and maintain a higher level of independence and comfort.
Expected Outcome of Generalized Osteoarthritis
The expected outcome of generalized osteoarthritis varies greatly depending on several factors, including the individual’s overall health, the severity of the condition, and the chosen treatment plan. Some individuals may experience only mild discomfort and minimal functional limitations, while others may face more significant challenges. In general, the progression of generalized osteoarthritis is often gradual, with symptoms worsening over time if not managed properly.
Maintaining a healthy lifestyle, including regular exercise and a balanced diet, plays a critical role in slowing the progression and improving the overall outcome. Early intervention and adherence to treatment recommendations are key to managing the condition effectively and preventing severe complications.
Potential Complications Associated with Generalized Osteoarthritis
Generalized osteoarthritis can lead to a range of complications, affecting various aspects of daily life. These complications often stem from the progressive deterioration of cartilage and bone, leading to joint instability, pain, and reduced mobility. Addressing these complications promptly is vital for preventing long-term disability and maintaining a good quality of life.
- Joint Deformities: Progressive cartilage loss and bone remodeling can result in visible joint deformities, impacting both aesthetics and functionality. These deformities may include joint instability, subluxation, and the development of bony spurs, commonly referred to as osteophytes.
- Chronic Pain and Stiffness: Persistent pain and stiffness in multiple joints can significantly impair daily activities, impacting mobility, work productivity, and social interactions. Chronic pain can also negatively impact mental health, potentially leading to depression or anxiety.
- Reduced Mobility and Functional Limitations: The progressive loss of joint function in multiple joints can significantly limit mobility and independence. This can make simple tasks like walking, climbing stairs, or dressing challenging, impacting a person’s ability to perform everyday activities. For example, a person with severe generalized osteoarthritis might find it difficult to walk more than a few blocks without experiencing significant pain.
- Muscle Weakness and Atrophy: Chronic pain and limited use of affected joints can lead to muscle weakness and atrophy. This further reduces mobility and functional capacity, creating a vicious cycle that worsens over time. Proper exercise and physical therapy are essential to counteract this effect.
- Sleep Disturbances: Chronic pain and discomfort associated with generalized osteoarthritis can lead to significant sleep disturbances, further exacerbating the condition’s negative effects on overall health and well-being. A good sleep hygiene routine and pain management strategies can contribute to improved sleep quality.
Long-Term Effects of Generalized Osteoarthritis
The long-term effects of generalized osteoarthritis can be profound, impacting a person’s physical and mental well-being. The progressive nature of the disease can lead to significant disability and reduced quality of life if not managed effectively. Early diagnosis, consistent treatment, and proactive lifestyle adjustments are critical for minimizing long-term effects.
Preventative Measures to Reduce the Impact of Complications
Proactive measures can significantly reduce the risk of complications associated with generalized osteoarthritis. These measures focus on maintaining joint health, promoting overall well-being, and managing pain effectively. Regular exercise, maintaining a healthy weight, and adhering to a balanced diet contribute to overall joint health and can slow the progression of the disease.
- Regular Exercise: Maintaining a regular exercise routine, incorporating low-impact activities like swimming, cycling, or walking, is crucial for maintaining joint mobility and muscle strength. Consult with a physician or physical therapist to create a tailored exercise plan that aligns with individual needs and limitations.
- Weight Management: Maintaining a healthy weight significantly reduces stress on joints, slowing the progression of osteoarthritis. A balanced diet and regular exercise contribute to weight management.
- Proper Posture and Body Mechanics: Adopting proper posture and body mechanics when performing daily tasks can reduce strain on joints. Learning how to lift objects properly and maintaining good posture during activities can significantly reduce stress on affected joints.
- Adequate Joint Protection: Protecting joints from excessive stress and strain is essential. Using assistive devices, such as canes or walkers, can provide support and reduce the load on affected joints.
- Pain Management Strategies: Implementing effective pain management strategies, including medication, physical therapy, and alternative therapies, can significantly improve quality of life and reduce the risk of complications.
Potential Complications Summary
| Potential Complications | Severity Level (1-5, 1 being least severe, 5 being most severe) |
|---|---|
| Joint Deformities | 3-5 |
| Chronic Pain and Stiffness | 2-5 |
| Reduced Mobility and Functional Limitations | 3-5 |
| Muscle Weakness and Atrophy | 2-4 |
| Sleep Disturbances | 1-3 |
Note: Severity levels are estimates and can vary based on individual circumstances.
Generalized osteoarthritis is a broad term for the general wear and tear on joints throughout the body. It’s often a gradual process, but it can lead to significant pain and stiffness. Interestingly, some research suggests a possible link between certain vascular conditions, like spider angioma, and osteoarthritis in specific cases. To learn more about what a spider angioma is, check out this helpful resource: what is spider angioma.
However, it’s crucial to remember that generalized osteoarthritis isn’t directly caused by spider angiomas; they might be associated in some situations. Ultimately, understanding generalized osteoarthritis requires a multifaceted approach.
Illustrative Examples
Generalized osteoarthritis, while often associated with aging, can affect individuals of all ages and impact their lives in profound ways. Understanding the condition through real-life examples can offer valuable insight into its diverse presentations and the challenges faced by those living with it. These examples aim to highlight the variability of the condition and the importance of personalized care.
A Case Study of Generalized Osteoarthritis
A 55-year-old female, Sarah, presented with generalized joint pain and stiffness, impacting multiple joints simultaneously. Her symptoms initially manifested as mild aches in her hands, knees, and hips, progressing over several years. The pain was often exacerbated by activity and relieved by rest. Morning stiffness, lasting for over an hour, became a daily routine. Radiographic imaging revealed significant joint space narrowing and osteophyte formation across various joints, confirming a diagnosis of generalized osteoarthritis.
A Patient’s Journey with Generalized Osteoarthritis
Sarah’s journey with generalized osteoarthritis involved various stages and treatments. Initially, she employed over-the-counter pain relievers and lifestyle modifications, such as weight management and low-impact exercises. As the condition progressed, she transitioned to prescription pain medications and physical therapy. Regular appointments with her rheumatologist and ongoing monitoring were crucial for managing symptoms and preventing further deterioration. Joint replacement surgery was considered as a possible treatment option for her severely affected joints.
Progression of the Condition
The progression of generalized osteoarthritis is often gradual and variable. Initial symptoms may be mild, presenting as intermittent joint pain and stiffness. As the disease advances, symptoms become more persistent and severe, affecting daily activities. Joint mobility decreases, leading to limitations in range of motion and functional independence. Over time, structural changes in the joints become evident through imaging studies.
Patient Experience with Generalized Osteoarthritis
Sarah’s experience with generalized osteoarthritis involved significant disruptions to her daily life. Simple tasks like walking, climbing stairs, or even holding a cup became increasingly challenging. She reported fatigue and emotional distress associated with the chronic pain and limitations. Her social life was impacted, as she found it difficult to participate in activities she once enjoyed. Despite these challenges, Sarah maintained a positive outlook and actively engaged in managing her condition through various therapies.
Impact on Daily Activities
Generalized osteoarthritis significantly impacts daily activities. For example, tasks such as cooking, cleaning, and personal hygiene might become more time-consuming and difficult. The inability to perform daily tasks independently can lead to dependence on others for assistance. Mobility limitations can affect participation in social activities and leisure pursuits. A visual representation of this impact could be depicted by illustrating the reduced ability to perform common activities, such as walking a certain distance, carrying objects, or getting dressed.
Daily tasks that were once effortless now require considerable effort and time. The limitations progressively reduce independence and quality of life.
Final Wrap-Up
In conclusion, generalized osteoarthritis presents a significant health concern that impacts individuals in various ways. By understanding its multifaceted nature, from causes to potential complications, individuals can proactively manage the condition. We’ve explored the critical aspects of generalized osteoarthritis, equipping you with a comprehensive overview to better navigate this health challenge. Remember, proper diagnosis and personalized treatment strategies are crucial in effectively managing this condition.





