What is a colposcopy? It’s a procedure used to examine the cervix and vagina for abnormalities. This in-depth look delves into the purpose, patient populations, historical context, procedure, and potential complications associated with colposcopy. We’ll cover everything from preparation and patient experience to the interpretation of results and follow-up care. Get ready to learn all about this vital diagnostic tool!
This comprehensive guide provides a clear overview of the colposcopy procedure, outlining its various aspects from the initial patient consultation to the final interpretation of results. We’ll also touch on the different visualization techniques used, the potential complications, and the importance of post-procedure care.
Introduction to Colposcopy

Colposcopy is a medical procedure used to examine the cervix, vagina, and surrounding tissues. It’s a crucial tool for detecting abnormal cells that might indicate the presence of precancerous or cancerous conditions. This non-invasive procedure provides a magnified view of these areas, allowing doctors to identify potential issues early, promoting effective treatment and improved patient outcomes.The purpose of a colposcopy is to investigate unusual changes in the tissues of the lower genital tract.
These changes may be visible or suspected based on symptoms, screening tests, or risk factors. It aids in early diagnosis and allows for targeted biopsies if necessary, enabling prompt treatment and reducing the risk of progression to more serious conditions. The procedure helps to identify precancerous lesions, which, if left untreated, can develop into cervical cancer.
A colposcopy is a procedure where a doctor uses a special instrument to examine the cervix and vagina. It’s often used to check for abnormal cells, which can sometimes indicate early signs of cancer. While we’re on the topic of reproductive health, you might also be interested in learning more about alternative methods of male birth control, such as male birth control injections.
Ultimately, colposcopies are a crucial tool for women’s health, providing early detection and potential intervention.
Typical Patient Population
Women who are experiencing abnormal vaginal bleeding, abnormal Pap smear results, or have risk factors for cervical cancer are commonly candidates for colposcopy. This may include women with a history of sexually transmitted infections (STIs), multiple sexual partners, or a family history of cervical cancer. Age, although a risk factor, is not the sole determinant. A significant number of women in their reproductive years undergo this procedure.
Historical Context
Colposcopy’s development stemmed from the need for a more effective way to visualize the cervix and surrounding tissues. Early attempts involved using simple magnifying glasses, but these proved insufficient for detailed examination. The invention of the colposcope, a specialized microscope, revolutionized the procedure. This device, equipped with a light source and magnification capabilities, allowed for a comprehensive view of the tissues, facilitating the identification of abnormalities.
The advancement of colposcopy has led to significant improvements in the early detection and treatment of cervical abnormalities.
Steps of a Typical Colposcopy Procedure
A typical colposcopy procedure involves several key steps:
- The patient is positioned comfortably on an examination table, similar to a gynecological exam.
- The physician applies a topical antiseptic to the area to be examined.
- A speculum is inserted into the vagina to hold it open, allowing for clear visualization.
- The colposcope is then placed on the cervix, providing a magnified view of the tissue.
- The physician may use acetic acid or Lugol’s iodine solution to highlight abnormal cells.
- If necessary, a biopsy is taken to collect a tissue sample for further analysis under a microscope.
- Finally, the physician cleans the area and removes the speculum and colposcope.
Common Reasons for Performing a Colposcopy
The table below Artikels common reasons for performing a colposcopy, encompassing symptoms, risk factors, and diagnostic goals:
| Reason | Symptoms | Risk Factors | Diagnostic Goals |
|---|---|---|---|
| Abnormal Pap Smear | Abnormal vaginal bleeding (intermenstrual, post-coital, post-menopausal), unusual discharge | History of HPV infection, multiple sexual partners, family history of cervical cancer, smoking, weakened immune system | Identify and characterize abnormal cervical cells, assess for precancerous lesions |
| Persistent Abnormal Vaginal Bleeding | Intermenstrual bleeding, post-coital bleeding, postmenopausal bleeding | Use of hormonal contraceptives, history of STIs, certain medical conditions | Evaluate the source of bleeding, rule out malignancy, identify any structural abnormalities |
| Suspected Cervical Lesion | Pain or discomfort in the pelvic area, unusual vaginal discharge | History of cervical dysplasia, exposure to certain chemicals or irritants | Identify the nature of the lesion, assess its extent, and plan for appropriate treatment |
| Follow-up After Treatment | No specific symptom | Previous abnormal Pap smear, history of abnormal cervical findings | Assess the effectiveness of treatment, detect recurrence of abnormalities |
Procedure and Techniques
A colposcopy is a crucial diagnostic procedure for evaluating the cervix and vagina. It allows healthcare providers to visualize these areas in detail, enabling the identification of abnormal cells or tissues that might indicate precancerous or cancerous conditions. This detailed examination is often a follow-up step after abnormal Pap tests or other screenings. Understanding the procedure’s steps and the instruments involved is essential for both patients and healthcare professionals.The colposcopy procedure involves several key steps, from preparation to biopsy if necessary.
Proper preparation and the use of specialized instruments and techniques are essential to ensure accurate diagnosis and patient comfort.
Physical Preparation
Adequate preparation for a colposcopy ensures a clear view of the targeted areas. This typically involves refraining from douching, using vaginal creams, or having intercourse for a few hours before the procedure. The patient should inform the healthcare provider of any existing allergies or sensitivities to medications. Emptying the bladder before the procedure is often recommended to facilitate comfort and a clear examination area.
Instruments Used
A colposcope, a specialized instrument with a magnifying lens and a light source, is the primary tool in a colposcopy. It allows for a magnified view of the cervix and vagina. Other instruments, such as speculums, are used to hold the vaginal walls apart, providing a wider field of view. A variety of brushes, spatulas, and biopsy forceps are also used to collect samples for further examination.
These instruments are specifically designed for the procedure, ensuring both precision and safety.
Procedure and Visualization Techniques
The colposcopy procedure begins with the patient positioning themselves on the examination table in a lithotomy position. A speculum is inserted to hold the vaginal walls apart, allowing access to the cervix and vagina. The colposcope is then placed in position, providing a magnified view of the tissues. Different visualization techniques, such as acetic acid application and Lugol’s iodine solution, are used to highlight abnormalities.
Acetic acid application can cause abnormal cells to appear white, while Lugol’s iodine stains healthy tissue. This helps in differentiating normal from abnormal tissues, increasing diagnostic accuracy. Using these techniques allows the healthcare provider to visualize potential irregularities in detail.
Types of Colposcopy Procedures
Colposcopy procedures can vary based on the specific area being examined. For instance, a cervical colposcopy focuses on the cervix, while a vaginal colposcopy assesses the vaginal walls. In some cases, a biopsy is taken for further examination, particularly when suspicious lesions are identified.
Role of Biopsy in Colposcopy
If abnormal areas are detected during the colposcopy, a biopsy may be necessary. A biopsy involves taking a small tissue sample for laboratory analysis. This analysis helps determine if the abnormal cells are cancerous or precancerous. The biopsy procedure is usually performed under local anesthesia and is a crucial step in confirming or ruling out potential cancerous or precancerous conditions.
This further examination is essential for making an accurate diagnosis and guiding treatment plans.
A colposcopy is a procedure where a doctor uses a special instrument to examine the cervix and vagina. It’s often used to investigate unusual cells or abnormal tissue. Knowing the differences between cold remedies like Mucinex and DayQuil can be just as important as understanding this procedure, as some cold medicines can interact with other medications. For a deeper dive into the similarities and differences between Mucinex and DayQuil, check out this helpful comparison: mucinex vs dayquils similarities and differences.
Ultimately, understanding the details of a colposcopy can help you make informed decisions about your health.
Comparison of Colposcopy Visualization Techniques
| Technique | Advantages | Disadvantages | Applications |
|---|---|---|---|
| Acetic Acid Application | Highlights abnormal cells, simple to perform, cost-effective | May not detect all abnormalities, can be affected by vaginal discharge | Initial screening for abnormal cervical cells |
| Lugol’s Iodine Staining | Differentiates normal and abnormal tissues, enhances visualization of lesions | May not be as sensitive as acetic acid, requires appropriate expertise | Assessing for atypical squamous cells and identifying areas for biopsy |
Indications and Contraindications
Colposcopy, a crucial procedure in gynecological care, is not a one-size-fits-all approach. Understanding the specific reasons for its application and potential obstacles is paramount for patient safety and optimal outcomes. This section delves into the indications for performing a colposcopy, potential complications, and contraindications, providing a comprehensive overview.A thorough evaluation of a patient’s medical history, symptoms, and relevant diagnostic tests is essential to determine if colposcopy is the appropriate diagnostic tool.
This assessment guides the selection of appropriate procedures and minimizes potential risks.
Indications for Colposcopy
Identifying abnormal cervical or vaginal tissues is a key driver for colposcopy. Various factors can trigger this need, from abnormal Pap smears to persistent vaginal bleeding. Suspicion of precancerous or cancerous lesions significantly influences the decision to perform colposcopy. The aim is to accurately diagnose and manage conditions that could potentially lead to more serious health issues.
- Abnormal Pap smear results, particularly those indicating atypical squamous cells of undetermined significance (ASCUS), low-grade squamous intraepithelial lesions (LSIL), or high-grade squamous intraepithelial lesions (HSIL). These findings warrant further investigation to determine the nature and extent of the abnormality.
- Persistent vaginal bleeding, especially post-coital or post-menopausal bleeding, requires careful evaluation. Colposcopy can help identify underlying causes, such as polyps, cervical erosion, or cancerous growths.
- Genital warts or other sexually transmitted infections (STIs) can sometimes present with atypical cytological findings, prompting the need for colposcopy to rule out associated abnormalities.
- Post-partum or post-abortion bleeding can be indicative of cervical trauma or other issues that warrant colposcopic examination.
- Patients with a history of cervical dysplasia or cancer are frequently monitored with colposcopy to assess the extent of any residual or recurring lesions and evaluate treatment effectiveness.
Potential Complications of Colposcopy
While generally safe, colposcopy, like any medical procedure, carries potential risks. Understanding these complications is essential for informed decision-making.
A colposcopy is a procedure where a doctor uses a special instrument to examine the cervix and vagina. It’s often recommended for women experiencing unusual vaginal bleeding or other concerning symptoms. Thinking about healthy choices, have you ever wondered about the potential health effects of palm oil? It’s a topic worth exploring. Learning more about the potential impacts of palm oil on health can be really helpful when making dietary decisions.
Ultimately, a colposcopy is a vital tool in women’s health care, helping to detect and address potential issues early. is palm oil bad for you
- Bleeding is a common complication, though usually minor and easily managed. Severe bleeding, however, can occur and necessitate further intervention, such as cauterization or other hemostatic measures.
- Infection is a potential risk, though it is usually preventable with appropriate infection control measures. Prompt recognition and treatment are crucial.
- Cervical lacerations or perforation are possible, although rare. Proper technique and careful monitoring minimize these risks.
- Post-procedure discomfort, such as cramping or pelvic pain, is a possible side effect and typically resolves within a few days.
Contraindications to Colposcopy
Contraindications are situations where performing colposcopy is either inadvisable or medically impossible. These can be categorized for easier understanding.
- Active Pelvic Infections: Colposcopy should be postponed if the patient has an active pelvic inflammatory disease (PID) or other active infection to prevent the spread of infection and ensure optimal healing.
- Acute or Unstable Medical Conditions: Colposcopy may be postponed if the patient has a severe or unstable medical condition that could compromise their safety during or after the procedure, such as uncontrolled hypertension or cardiac instability.
- Active Vaginal Bleeding: Significant and uncontrolled vaginal bleeding may create complications during the procedure and may also contraindicate colposcopy, necessitating management of the bleeding first.
Comparison of Indications
The indications for colposcopy often overlap. For example, abnormal Pap smears and post-coital bleeding might both lead to a colposcopy. However, the specific concern, the extent of abnormality, and the patient’s history differentiate the cases. A careful clinical judgment is necessary to determine the most appropriate course of action.
Contraindications Summary Table
| Indication | Description | Risk Assessment | Further Evaluation |
|---|---|---|---|
| Abnormal Pap Smear (ASCUS, LSIL, HSIL) | Suggests precancerous or cancerous cervical lesions. | Low risk of complications if performed appropriately. | Further testing (e.g., HPV testing) to determine the cause and severity of the abnormality. |
| Persistent Vaginal Bleeding | Ongoing bleeding, especially post-coital or post-menopausal. | Moderate risk of complications if bleeding is significant. | Assessment of the source of bleeding through imaging or other tests. |
| Active Pelvic Infection | Presence of active PID or other infection. | High risk of complications if performed during infection. | Treatment of the infection before proceeding with colposcopy. |
| Uncontrolled Hypertension | Uncontrolled blood pressure. | Increased risk of complications during and after procedure. | Control of blood pressure prior to colposcopy. |
Interpreting Results and Follow-up
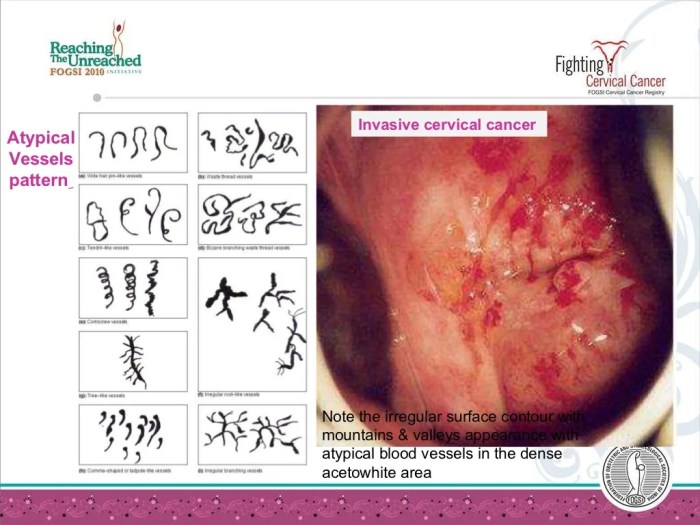
Deciphering the results of a colposcopy is crucial for determining the appropriate course of action. This stage involves careful analysis of the visual findings and associated tissue samples, leading to an accurate diagnosis and tailored treatment plan. A thorough understanding of the implications of different findings is essential for both the patient and the healthcare provider.Proper follow-up care after a colposcopy is equally vital.
This encompasses regular check-ups, potentially involving further diagnostic procedures or treatments, to monitor the condition and ensure the best possible outcome. A proactive approach to follow-up minimizes the risk of complications and promotes overall well-being.
Colposcopy Result Interpretation
Colposcopy results are interpreted by comparing the observed findings with established diagnostic criteria. Visual characteristics such as color, texture, size, and location of any abnormalities are meticulously documented. Histopathological analysis of tissue samples obtained during the procedure provides crucial insights into the cellular structure and potential malignancy. Experienced gynecologists and pathologists use this combination of visual and microscopic data to arrive at a diagnosis.
Importance of Follow-up Care
Follow-up care after a colposcopy is essential for monitoring the progression of any identified abnormalities. Regular check-ups allow for early detection of potential complications and enable prompt intervention if necessary. These appointments also provide opportunities to discuss any concerns and address patient questions regarding the results and their implications. Patient compliance with follow-up recommendations is critical for effective management of the condition.
Typical Colposcopy Findings and Implications
Various findings can be observed during a colposcopy. Abnormal cells or tissues might present as lesions, discolorations, or unusual textures. The location and extent of these abnormalities significantly influence the potential diagnosis and subsequent treatment.
Possible Diagnoses from Colposcopy
Colposcopy can lead to a range of diagnoses, from benign conditions to precancerous lesions or even cervical cancer. The interpretation considers the totality of the findings, including visual observations and microscopic analysis of tissue samples. Examples of diagnoses derived from colposcopy include cervical intraepithelial neoplasia (CIN), atypical squamous cells of undetermined significance (ASCUS), and low-grade squamous intraepithelial lesions (LSIL).
Treatment Options Based on Colposcopy Results
Treatment options depend on the specific diagnosis and the severity of the condition. Treatment options might include watchful waiting, cryotherapy, laser therapy, or surgical excision, depending on the specific condition. In cases of more severe abnormalities, referral to a specialist or further diagnostic procedures may be necessary.
Table of Typical Colposcopy Findings and Treatment
| Finding | Description | Possible Diagnosis | Treatment Options |
|---|---|---|---|
| Abnormal Cervical Lesion (e.g., CIN 1) | Small, reddish, or white area on the cervix | Cervical Intraepithelial Neoplasia Grade 1 | Often observed with watchful waiting and repeat colposcopies; further treatments may include cryotherapy or laser therapy |
| Large, irregular lesion on cervix | Large, irregular area with abnormal vascular patterns and visible tissue distortion | Cervical Intraepithelial Neoplasia (CIN 2 or 3) | Surgical excision (e.g., cone biopsy), cryotherapy, or laser therapy; the specific treatment depends on the severity of the lesion and patient factors. |
| Normal Cervix | Healthy cervix with no visible abnormalities | No significant abnormalities | Routine follow-up and monitoring for future check-ups. |
Patient Experience and Preparation
Navigating a colposcopy can be a nerve-wracking experience for many women. Understanding the procedure, preparation, and potential anxieties associated with it can significantly ease apprehension and promote a more comfortable experience. This section will Artikel the patient experience, preparation guidelines, and the crucial role of education in managing anxieties related to this important diagnostic procedure.A colposcopy is a relatively straightforward procedure, but the experience can vary from patient to patient.
Many patients report feeling a sense of nervousness or apprehension before the procedure. Effective patient preparation, education, and clear communication from healthcare providers are vital in mitigating these anxieties and fostering a positive experience.
Patient Experience During the Procedure
The colposcopy procedure itself typically lasts between 15 and 30 minutes. Patients are seated during the examination, and a speculum is used to visualize the cervix. A vinegar solution or other staining agents may be applied to the cervix to highlight any abnormalities. A colposcope, a specialized microscope, is then used to magnify the area and allow the healthcare provider to examine it more closely.
In some cases, a biopsy may be taken for further analysis. The overall experience is generally described as being somewhat uncomfortable but not painful.
Patient Preparation and Pre-Procedure Instructions, What is a colposcopy
Proper preparation is essential for a successful colposcopy. Patients should follow specific instructions provided by their healthcare provider. These may include avoiding certain medications (like aspirin or ibuprofen) and foods that can increase bleeding, as well as refraining from sexual activity for a certain period before the procedure.
Role of Patient Education in Colposcopy Preparation
Patient education plays a critical role in preparing for a colposcopy. Healthcare providers should thoroughly explain the procedure, its purpose, and the potential outcomes. Open communication and answering any questions or concerns can significantly alleviate anxiety. Explaining the procedure step-by-step, the reason for the procedure, and the potential results of the testing will empower the patient to face the process with confidence.
Potential Anxieties Associated with Colposcopy
Fear of the unknown, discomfort during the procedure, and concerns about the potential results are common anxieties associated with colposcopy. Open communication, reassurance, and detailed explanations about the procedure and its significance can help alleviate these concerns. Providing clear and concise information about the steps involved and the expected outcomes can reduce anxiety and promote a more positive patient experience.
Step-by-Step Guide for Preparing for a Colposcopy
This structured guide helps patients understand the preparation process for a colposcopy. A patient-friendly and easily accessible format can ensure the procedure is carried out with minimal stress.
- Consult with your healthcare provider: Discuss any concerns or questions you may have about the procedure, including the necessity, risks, benefits, and alternatives. This initial step is crucial in alleviating anxieties and building trust with your healthcare provider.
- Follow pre-procedure instructions: Your healthcare provider will provide specific instructions about what to do and avoid before the procedure. This might include refraining from certain medications, foods, or activities.
- Arrange transportation: If necessary, arrange for transportation to and from the appointment, as you may not feel your best after the procedure.
- Inform your support system: Let someone know about your appointment, and if possible, ask for their support before, during, and after the procedure. Having a support system can make the experience more manageable.
- Relax and stay calm: Deep breathing exercises or meditation can help manage anxiety. Engage in activities you enjoy, such as reading or listening to music, to distract from the upcoming procedure.
Important considerations for a successful colposcopy include meticulous adherence to pre-procedure instructions, open communication with your healthcare provider, and proactive management of any anxieties or concerns. A well-informed and prepared patient is better equipped to navigate the procedure and contribute to a positive outcome.
Safety and Risks: What Is A Colposcopy
Colposcopy, while a crucial procedure for diagnosing cervical abnormalities, carries potential risks. Understanding these risks and the safety precautions taken is essential for both patients and healthcare providers. This section details the safety measures employed during the procedure, potential complications, and post-procedure care to ensure a positive and safe experience.
Safety Precautions During Colposcopy
Strict adherence to safety protocols is paramount during colposcopy. These protocols are designed to minimize risks and ensure the well-being of the patient. Proper sterilization techniques for instruments and equipment are critical to prevent infections. Aseptic technique, encompassing meticulous handwashing and the use of sterile drapes and gloves, is implemented throughout the procedure. Maintaining a sterile field around the patient is also essential.
Additionally, the equipment used, including the colposcope itself, is meticulously cleaned and sterilized between procedures to prevent cross-contamination.
Potential Risks and Complications
Various potential risks and complications, although rare, can arise during or after a colposcopy. These risks are categorized for clarity.
Bleeding
Bleeding is a common potential complication, although usually minor and easily controlled. The procedure involves dilation of the cervix and the application of acetic acid or other substances, which can temporarily increase the risk of bleeding. Post-procedure bleeding can be a concern, but it’s generally manageable.
Infection
Infection is a risk associated with any invasive procedure. Strict adherence to aseptic technique minimizes the risk, but it’s still possible. Symptoms of infection may include fever, unusual vaginal discharge, or increased pain. Prompt medical attention is crucial if these symptoms develop.
Cervical Trauma
The use of instruments during colposcopy, including the speculum and biopsy forceps, can potentially cause minor trauma to the cervix. While often insignificant, significant trauma is rare. Care is taken to minimize this risk through gentle handling of the cervix and appropriate instrument selection.
Vaginal or Pelvic Pain
Some discomfort or pain is common during and after colposcopy, usually mild and temporary. However, persistent or severe pain requires immediate evaluation by a healthcare provider.
Complications from Biopsy
If a biopsy is taken, there is a slight risk of complications. These include bleeding, infection, or discomfort at the biopsy site.
Post-Procedure Care
Proper post-procedure care is essential to promote healing and prevent complications. Patients are typically advised to avoid strenuous activity and heavy lifting for a day or two after the procedure. Maintaining good hygiene practices, such as using a mild cleanser for the affected area and avoiding douching, is vital. Patients should be informed about signs to watch for and when to seek medical attention.
Mitigation Strategies
Several strategies can mitigate the potential risks associated with colposcopy. These strategies involve meticulous attention to detail, appropriate instrument selection, and close monitoring of the patient throughout the procedure.
Table of Safety Procedures and Potential Risks
| Procedure | Safety Measures | Potential Risks | Mitigation Strategies |
|---|---|---|---|
| Colposcopy | Strict adherence to aseptic technique, sterile instruments, meticulous handwashing | Bleeding, infection, cervical trauma, vaginal or pelvic pain | Gentle handling of instruments, careful monitoring, prompt management of any complications |
| Biopsy (if performed) | Precise biopsy technique, careful tissue handling | Bleeding, infection, discomfort at biopsy site | Minimizing the size and depth of biopsy, appropriate wound care |
Final Review
In conclusion, colposcopy is a crucial procedure for detecting and managing potential gynecological issues. Understanding the process, from preparation to interpretation of results, is vital for both patients and healthcare providers. By comprehending the different techniques, indications, and possible complications, we can ensure the best possible outcomes for those undergoing this examination. Remember, open communication with your healthcare provider is key to navigating the entire colposcopy journey.




