Tinea nigra symptoms causes diagnosis is crucial for accurate identification and effective treatment. This condition, often appearing as a dark, discolored patch on the skin, requires a thorough understanding of its various aspects. We’ll explore the key symptoms, delve into potential causes, and examine the diagnostic procedures used by healthcare professionals.
From the initial appearance to the various treatment options, this comprehensive guide will walk you through the nuances of tinea nigra. Understanding the visual characteristics, the underlying fungal culprits, and the diagnostic steps will empower you with a deeper insight into this skin condition. This detailed approach ensures a complete understanding of tinea nigra, empowering you with knowledge to better navigate the medical process.
Introduction to Tinea Nigra
Tinea nigra is a common, benign fungal infection of the skin. It’s characterized by the appearance of dark, often slightly raised, macules on the skin. While not a serious health concern, it can be cosmetically unappealing and may cause mild discomfort for some individuals. This fungal infection is relatively easy to treat, and early detection often leads to a rapid resolution.This condition is often misidentified, as the appearance can resemble other skin conditions.
Understanding its characteristics, including typical symptoms, affected areas, and prevalence, is crucial for proper diagnosis and treatment. It’s important to note that while often a straightforward diagnosis, it’s best to consult a healthcare professional for accurate identification and appropriate treatment.
Common Names and Synonyms
Tinea nigra is also known by various names, including “black fungus” and “black skin infection”. These terms reflect the distinctive dark pigmentation of the lesions. These alternative names are sometimes used in everyday conversations, but it’s crucial to remember that Tinea nigra is a specific medical term.
Affected Areas
Tinea nigra lesions are most frequently found on the palms of the hands and soles of the feet. Occasionally, it may appear on other areas of the body. The areas most often affected are those that are frequently exposed to moisture and humidity. This suggests that environmental factors play a role in the development of the infection.
Prevalence and Demographics
Tinea nigra is a relatively common fungal infection, particularly in tropical and subtropical regions. Individuals living in these areas may experience a higher prevalence of the condition. The infection can occur in people of all ages and ethnic backgrounds, but its prevalence might be slightly higher in certain demographic groups. The frequency is influenced by factors such as climate and hygiene practices.
Appearance of Lesions
The characteristic lesion of tinea nigra is a dark, brown, or black macule, or slightly raised area. The colour can vary depending on the individual. The lesion is typically flat and well-defined. These lesions may range in size from a few millimeters to several centimeters in diameter. The appearance is often compared to a slightly raised, dark spot on the skin.
Initial Symptoms
| Symptom | Description |
|---|---|
| Dark macules | Small, flat, dark spots on the skin, often appearing brown or black. |
| Slightly raised lesions | The lesions may be slightly elevated above the surrounding skin, giving a subtle bump-like appearance. |
| Asymptomatic | In many cases, tinea nigra is asymptomatic, meaning there are no noticeable symptoms beyond the visible lesion. |
Symptoms of Tinea Nigra: Tinea Nigra Symptoms Causes Diagnosis
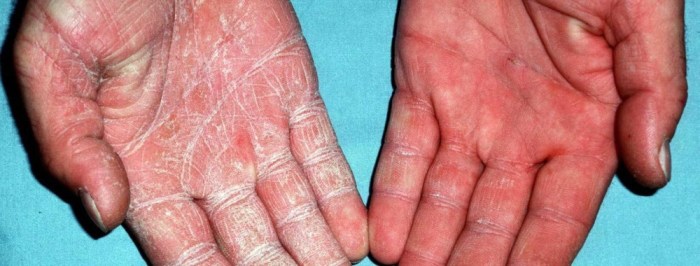
Tinea nigra, a fungal infection of the skin, presents with distinctive visual characteristics that can help in its identification. Understanding these symptoms is crucial for early diagnosis and appropriate treatment. Early recognition can prevent the infection from spreading and ensure a quicker recovery.Identifying the telltale signs of tinea nigra is essential for prompt medical intervention. The key is to pay attention to the visual clues, including the specific color, texture, and size of the lesions.
By familiarizing yourself with these visual characteristics, you can better distinguish this condition from other skin ailments.
Visual Characteristics of Lesions
The hallmark of tinea nigra is the presence of dark-colored, flat, and slightly raised lesions on the skin. These lesions typically appear as macules, which are flat spots on the skin, and are not elevated or bumpy. They are often mistaken for other skin discolorations.
Figuring out tinea nigra symptoms, causes, and diagnosis can be tricky. It’s often a harmless skin discoloration, but knowing the details helps in proper identification. Understanding the different phases of healing, like those for a c section scar c section scar healing stages , can provide insight into how skin conditions manifest and resolve. Ultimately, proper diagnosis for tinea nigra relies on a combination of visual inspection and potentially a skin scraping for analysis.
Color and Texture of Lesions
The color of tinea nigra lesions is typically dark brown to black, which is the source of its name. The texture is usually smooth and somewhat waxy, though the description may vary. The shade can range from a light brownish-gray to a very dark brown or black, depending on the individual’s skin tone and the extent of the infection.
The color difference from the surrounding skin is usually significant.
Size and Shape of Lesions
Tinea nigra lesions typically range in size from a few millimeters to a few centimeters in diameter. The shape of the lesions is often oval or irregular. They are usually well-defined, meaning the edges of the lesion are distinct and separate from the healthy skin. Lesions can also appear in clusters, though individual lesions tend to have a solitary presence.
Associated Symptoms
In many cases, tinea nigra does not cause any significant associated symptoms, such as itching or pain. However, some individuals may experience mild irritation or a feeling of dryness in the affected area. It is important to note that the absence of itching or pain does not rule out the presence of the infection.
Symptom Summary Table
| Symptom | Description | Severity |
|---|---|---|
| Color | Dark brown to black, noticeable against surrounding skin | Mild |
| Texture | Smooth, waxy | Mild |
| Size | A few millimeters to a few centimeters in diameter | Mild |
| Shape | Oval or irregular | Mild |
| Associated Symptoms | Mild irritation or dryness, often absent | Mild (or absent) |
Variations in Symptoms
Individual responses to tinea nigra can vary. While the characteristic dark coloration is often present, the severity and extent of the infection can differ from person to person. Factors such as the individual’s immune system and the specific strain of fungus can influence the symptoms experienced. For example, some individuals might have larger lesions or more extensive areas of involvement compared to others.
Causes of Tinea Nigra
Tinea nigra, a harmless but unsightly skin discoloration, is primarily caused by a specific type of fungus. Understanding the causative agents, transmission methods, and environmental influences is crucial for prevention and effective management. This section delves into the fungal species responsible, typical modes of transmission, and the role of environmental factors in infection.The culprit behind tinea nigra is a fungus belonging to the
- Hortaea werneckii* species, previously known as
- Exophiala werneckii*. This particular fungus thrives in warm, humid environments, and is often found in tropical and subtropical regions. It’s important to note that this fungus is not typically associated with severe health complications.
Fungal Species and Transmission
The fungusHortaea werneckii* is the primary causative agent of tinea nigra. This dimorphic fungus exists in both a yeast and a hyphal form, adapting to different environmental conditions. The fungal species is known to colonize keratinized tissues, like the skin. The infection typically develops in areas exposed to moisture, such as the hands and feet.
Mode of Transmission and Risk Factors
Tinea nigra is primarily acquired through indirect contact. This means the fungus isn’t usually passed directly from person to person via touch. Instead, the fungus thrives in damp environments, like humid bathrooms, locker rooms, or pools. Exposure to these contaminated surfaces can lead to infection.Risk factors for developing tinea nigra are often related to increased exposure to damp environments or conditions that promote fungal growth.
Individuals living in tropical or subtropical climates may be more susceptible due to the prevalence of humid conditions that support fungal growth.
Environmental Factors in Infection
Environmental factors play a crucial role in the development and transmission of tinea nigra. High humidity and warm temperatures are ideal conditions for the growth and proliferation of theHortaea werneckii* fungus. This is why the condition is often more prevalent in tropical and subtropical areas. Indirect contact with contaminated surfaces, like shower floors, is a common route of infection.
Direct vs. Indirect Contact
While direct contact isn’t the primary mode of transmission for tinea nigra, it’s still possible. Direct contact, like touching an infected person’s skin, might contribute in rare instances. However, indirect contact with contaminated surfaces is the more common and significant factor. This emphasizes the importance of hygiene and maintaining a clean environment to prevent the spread of the fungus.
Fungal Growth Conditions and Infection Factors
| Cause | Explanation |
|---|---|
| Warm, humid environments | These conditions are optimal for the growth and survival of the
|
| Indirect contact with contaminated surfaces | Exposure to surfaces harboring the fungus, such as shower floors or damp areas, increases the risk of infection. |
| Compromised skin barrier | In some cases, skin that is already damaged or compromised might be more susceptible to fungal colonization. |
TheHortaea werneckii* fungus thrives in environments with high humidity and warmth. Factors like the presence of moisture on the skin and compromised skin integrity can also contribute to infection. These conditions allow the fungus to colonize the skin and lead to the characteristic brown, black, or gray macules.
Diagnosis of Tinea Nigra
Tinea nigra, a relatively benign skin condition, is often diagnosed based on a combination of clinical findings and sometimes, laboratory tests. Accurate diagnosis is crucial for appropriate treatment and to rule out other, potentially more serious, conditions. A thorough understanding of the diagnostic process empowers both patients and healthcare providers in making informed decisions.
Physical Examination
A crucial aspect of diagnosing tinea nigra involves a careful physical examination. The characteristic dark, brownish-black, macules are typically the first sign. The physician will visually inspect the affected area for size, shape, and distribution of the lesions. Observing the borders, which are often well-defined, is also essential. Texture assessment, noting if the lesions feel smooth or slightly rough, provides additional information.
The presence or absence of scaling or inflammation is another important factor to consider. The physician will also check for any associated symptoms, such as itching or pain, which could help distinguish it from other skin conditions.
Medical History
A detailed medical history is vital in the diagnostic process. Information regarding recent travel, exposure to potential sources of infection, and any pre-existing skin conditions are relevant. For example, a history of recent travel to tropical regions could be a contributing factor in the development of tinea nigra. Any history of similar conditions in family members can also provide valuable insight.
Knowledge of any concurrent illnesses or medications the patient is currently taking is equally important. The physician will carefully gather this information to understand the potential contributing factors.
Dermatological Examination
A comprehensive dermatological examination, often employing a dermatoscope, can further aid in the diagnosis. The dermatoscope allows for a magnified view of the skin, enabling the physician to scrutinize the lesion’s structure and characteristics in greater detail. This detailed examination can help in distinguishing tinea nigra from other skin conditions with similar appearances. This step can identify fine details and patterns that may be missed during a routine visual inspection.
A dermascope is especially useful for assessing pigmentation and skin texture.
Importance of Images
High-quality images, ideally digital photographs, of the affected area are valuable tools in the diagnostic process. These images can be used for future comparisons and documentation of the condition’s progression. Photographs provide a permanent record of the lesion’s appearance, which is helpful for monitoring treatment response and evaluating the overall condition’s evolution. The images can be compared with previous images taken over time to show the effects of treatment.
The photographs can also be used to educate the patient about their condition.
Skin Scrapings and Laboratory Tests
Skin scrapings, taken from the affected area, are often sent to a laboratory for microscopic examination. This examination helps confirm the presence of the causative fungus,Hortaea werneckii*, and rule out other similar fungal infections. This technique is particularly useful for confirmation. A potassium hydroxide (KOH) preparation is a common laboratory procedure for microscopic visualization of fungal elements.
Additional laboratory tests, such as fungal cultures, might be necessary in some cases for a definitive diagnosis, especially when distinguishing between similar conditions.
Differentiation from Other Conditions
| Procedure | Description | Significance |
|---|---|---|
| Visual Inspection | Careful observation of the lesion’s appearance, including color, size, shape, and distribution. | Initial screening for characteristic features of tinea nigra. |
| Dermatoscopic Examination | Magnified view of the skin lesion using a dermatoscope. | Detailed evaluation of the lesion’s structure and characteristics for distinguishing it from other conditions. |
| KOH Preparation | Microscopic examination of a skin scraping stained with potassium hydroxide. | Confirmation of the presence of fungal elements, aiding in differentiating tinea nigra from other conditions. |
Tinea nigra can be easily confused with other skin conditions, like pityriasis versicolor or other pigmented skin lesions. A careful differential diagnosis, considering the patient’s medical history, physical examination findings, and laboratory results, is essential for accurate identification. For instance, pityriasis versicolor may exhibit similar pigmentation but typically presents with a more diffuse distribution and scaling. Differentiating these conditions is vital for accurate treatment.
Treatment Options for Tinea Nigra
Tinea nigra, a superficial fungal infection, typically responds well to treatment. Effective management focuses on eliminating the fungus and preventing recurrence. Prompt and appropriate treatment can significantly reduce the unsightly appearance and discomfort associated with the condition.Effective treatment for tinea nigra usually involves topical antifungal agents. These medications target the fungus directly, disrupting its growth and propagation.
The choice of treatment often depends on the severity of the infection, the individual’s response to treatment, and potential side effects.
Typical Treatment Strategies
Topical antifungal medications are the cornerstone of treatment for tinea nigra. These medications are applied directly to the affected skin. The selection of the appropriate topical agent is crucial for effective treatment. Different formulations, such as creams, ointments, and powders, offer varying degrees of penetration and efficacy.
Examples of Topical Medications
Several antifungal agents are commonly used to treat tinea nigra. Commonly prescribed topical medications include clotrimazole, miconazole, and ketoconazole. These agents exhibit varying degrees of antifungal activity, and their efficacy may vary depending on the individual. It is essential to follow the prescribed dosage and duration of treatment to ensure successful resolution.
Role of Antifungal Creams, Ointments, and Powders
Antifungal creams, ointments, and powders work by disrupting the fungal cell membrane or inhibiting fungal enzyme function. This interference prevents the fungus from multiplying, ultimately leading to the clearing of the infection. The choice between a cream, ointment, or powder often depends on the individual’s preference and the characteristics of the affected area. Creams are typically used for widespread areas, while ointments might be preferred for areas with cracks or fissures.
Powders are suitable for areas prone to moisture.
Potential Side Effects of Various Treatment Options
While topical antifungal medications are generally well-tolerated, some individuals may experience mild side effects. These can include skin irritation, redness, itching, or burning at the application site. The severity of these side effects varies among individuals and is often dependent on the specific medication used. It is crucial to monitor for any adverse reactions and to discontinue use if significant discomfort arises.
Consult a healthcare professional if the side effects persist or worsen.
Comparison of Treatment Approaches
Different topical antifungal agents may have varying mechanisms of action and potential side effects. The choice of treatment should be guided by factors such as the specific type of fungus involved, the severity of the infection, and the patient’s overall health. Careful consideration of the potential benefits and risks of each treatment is essential for optimal patient care.
How to Use Antifungal Creams Effectively
Proper application of antifungal creams is crucial for achieving optimal results. Clean and dry the affected area thoroughly before application. Apply a thin layer of the cream to the affected area, ensuring complete coverage. Follow the prescribed dosage and frequency of application diligently. Avoid using excessive amounts of the cream, as this can increase the risk of side effects.
Cover the area with a bandage if necessary. Keep the area clean and dry to promote healing.
| Treatment | Mechanism of Action | Potential Side Effects |
|---|---|---|
| Clotrimazole | Disrupts fungal cell membranes | Skin irritation, redness, itching, burning |
| Miconazole | Inhibits fungal enzyme function | Skin irritation, redness, itching, burning |
| Ketoconazole | Inhibits fungal growth | Skin irritation, redness, itching, burning, allergic reactions in some cases |
Prevention of Tinea Nigra
Preventing tinea nigra involves a proactive approach focusing on maintaining good hygiene and avoiding factors that contribute to the fungal infection’s growth. By understanding the environmental and personal habits that influence the development of this condition, individuals can significantly reduce their risk of contracting it.
Preventative Measures
Effective prevention hinges on a multi-faceted strategy encompassing various aspects of personal care and environmental control. Consistent adherence to these measures can significantly reduce the chances of developing tinea nigra.
- Maintaining Good Hygiene Practices: Regular and thorough cleansing of affected areas, especially feet, is crucial. This involves washing the affected skin with mild soap and water, ensuring complete removal of sweat and debris. Proper drying, particularly between toes and in skin folds, is equally important to prevent moisture buildup. Frequent bathing or showering, especially during periods of increased sweating, can help control moisture levels and limit fungal growth opportunities.
- Proper Foot Care and Moisture Control: Maintaining dry feet is a key preventative measure. Wearing breathable footwear that allows air circulation is essential. Using foot powders or antiperspirants can help absorb moisture and prevent fungal growth. If you have sweaty feet, consider using absorbent socks made of moisture-wicking materials. Regularly checking your feet for any signs of cracking, redness, or itching is vital to catch potential problems early.
Ever wondered about those dark, flat spots on your skin? Tinea nigra, a fungal infection, often shows up as these. Understanding its symptoms, causes, and diagnosis is key. Fortunately, similar to the meticulous preparation for shock therapy procedures, as detailed in this helpful resource on shock therapy process preparation outcomes and more , a proper diagnosis requires careful examination and testing to rule out other skin conditions.
So, if you’re experiencing these symptoms, seeking professional medical help is the best way to ensure the correct diagnosis and treatment plan.
- Avoiding Sharing Personal Items: Sharing personal items like towels, socks, and shoes should be avoided. This practice helps prevent the transmission of fungi from one person to another. Each individual should have their own personal items to avoid potential contamination.
- Maintaining Clean Environments: Regular cleaning of areas prone to moisture buildup, such as showers and bathrooms, is crucial. This helps to eliminate fungal spores and prevent their spread. Ensuring adequate ventilation in these areas is also beneficial.
- Avoiding Prolonged Exposure to Humid Conditions: Excessive humidity can create an environment conducive to fungal growth. Minimizing exposure to humid environments, such as by wearing appropriate clothing and footwear, can reduce the risk of tinea nigra.
Strategies for Prevention, Tinea nigra symptoms causes diagnosis
Implementing preventative strategies is a proactive measure to reduce the risk of developing tinea nigra. Consistent adherence to these strategies is crucial for successful prevention.
| Prevention Strategy | Explanation |
|---|---|
| Maintaining Good Hygiene | Regular cleansing of affected areas, especially feet, with mild soap and water, and thorough drying is essential. Frequent bathing or showering during periods of sweating can limit moisture buildup. |
| Proper Foot Care | Wearing breathable footwear, using foot powders or antiperspirants, and wearing moisture-wicking socks can help maintain dry feet and prevent fungal growth. |
| Avoiding Sharing Personal Items | Avoid sharing towels, socks, shoes, and other personal items to prevent the transmission of fungi. |
| Maintaining Clean Environments | Regular cleaning of areas prone to moisture buildup, such as showers and bathrooms, helps eliminate fungal spores. |
| Avoiding Humid Conditions | Minimizing exposure to humid environments can reduce the risk of tinea nigra, especially in areas where humidity is high. |
Visual Representation of Tinea Nigra
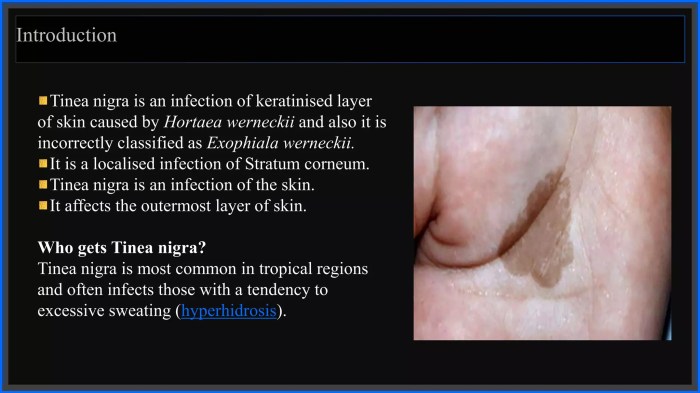
Tinea nigra is a fungal infection that primarily affects the skin, often appearing as a dark, discolored patch. Understanding its visual presentation is crucial for accurate diagnosis and appropriate treatment. This section delves into the characteristic appearance of tinea nigra lesions at various stages of development, highlighting differences across skin tones, and emphasizing the importance of visual aids in the diagnostic process.Visual identification of tinea nigra lesions is often the first step in diagnosis.
The dark, macule-like spots can easily be confused with other skin conditions, making visual clarity vital. Accurate diagnosis is essential for initiating the right treatment plan and preventing potential complications.
Typical Appearance of Lesions
The initial appearance of tinea nigra lesions is usually subtle, often presenting as a flat, dark macule. This macule’s color varies depending on the individual’s skin tone. Over time, the lesion may enlarge and darken, and its edges can become slightly irregular. The characteristic dark color of the lesion is a crucial distinguishing feature, as it helps differentiate it from other skin conditions that might have similar appearances.
Visual Representation Across Skin Tones
Tinea nigra’s visual presentation can differ slightly depending on the skin tone of the affected individual. On lighter skin tones, the lesion often appears as a dark brown or black macule. On darker skin tones, the lesion might appear as a slightly less distinct, dark brown or even bluish-gray macule. This variation is crucial to consider, as a misinterpretation could lead to an inaccurate diagnosis.
It’s essential for healthcare professionals to be aware of these variations and to use additional diagnostic tools where necessary.
Figuring out tinea nigra, with its distinctive dark spots, can be a bit of a puzzle. Understanding the symptoms, causes, and diagnosis is key, but sometimes, dealing with health concerns can trigger feelings of depression. Fortunately, developing good coping skills can be incredibly helpful in navigating those challenges. Learning strategies for managing stress and improving your mental well-being can make a significant difference in your overall health journey, as demonstrated by resources like coping skills for depression.
Ultimately, while tackling the physical aspects of tinea nigra, don’t forget to prioritize your mental health too. Seeking a proper diagnosis for tinea nigra is still the most important step to resolving this skin condition.
Importance of Visual Representations in Diagnosis
Visual representations, including photographs and illustrations, play a vital role in the diagnosis of tinea nigra. They provide a clear and objective record of the lesion’s appearance, enabling healthcare professionals to compare it to typical presentations of the infection. This comparison facilitates a more accurate diagnosis, especially when combined with other clinical findings and potentially a fungal culture or KOH examination.
Table of Lesion Stages
The following table Artikels the typical visual progression of tinea nigra lesions. Note that these are generalized descriptions, and individual cases may vary.
| Stage | Visual Description |
|---|---|
| Early Stage | A small, flat, dark brown or black macule, barely noticeable. The edges may appear slightly irregular or ill-defined. |
| Intermediate Stage | The macule enlarges, becoming more distinct and darker in color. The edges might become slightly more irregular. |
| Late Stage | The lesion may continue to enlarge and darken, potentially exhibiting a slightly raised or scaly appearance. The borders may become more well-defined, but still irregular. |
Differential Diagnosis
Tinea nigra, while often a benign skin condition, can sometimes be mistaken for other skin issues. Accurate diagnosis is crucial to ensure the appropriate treatment and avoid unnecessary interventions. Differentiating tinea nigra from similar conditions requires careful consideration of symptoms, causes, and potential treatments. This section explores common conditions that mimic tinea nigra, highlighting the importance of a proper diagnosis.
Conditions Mimicking Tinea Nigra
Several skin conditions can present with similar pigmentation and superficial appearance to tinea nigra, making accurate differentiation challenging. Careful observation of the lesion’s characteristics and medical history are essential.
Comparison of Mimicking Conditions
| Condition | Distinguishing Features |
|---|---|
| Tinea Nigra |
|
| Lichen Planus |
|
| Ephelis (Freckles) |
|
| Melasma |
|
| Pityriasis Versicolor |
|
Importance of Accurate Diagnosis
Accurate diagnosis of tinea nigra is crucial for effective treatment and to rule out other underlying conditions. Misdiagnosis can lead to inappropriate treatments, prolong the condition, or potentially mask a more serious issue. A healthcare professional should be consulted for proper evaluation and diagnosis, ensuring the right course of action is taken. For example, if a patient is misdiagnosed with tinea nigra, but actually has melasma, the treatment for tinea nigra will not address the underlying cause of the skin discoloration.
This could potentially worsen the condition or result in unnecessary and ineffective treatments.
Closing Summary
In conclusion, understanding tinea nigra symptoms, causes, and diagnosis is vital for proper management. The detailed exploration of symptoms, causes, and diagnostic procedures, along with the different treatment options, provides a comprehensive understanding. Prevention strategies are also key, focusing on hygiene, environmental factors, and avoiding prolonged exposure to humidity. By combining these factors, you’ll be better equipped to address this skin condition effectively.




