Sigmoid diverticulitis effect on the colon and diagnosis is a critical aspect of understanding this common digestive issue. This condition involves inflammation of small pouches (diverticula) in the sigmoid colon, a crucial part of the large intestine. Understanding the causes, progression, diagnostic methods, and treatment options for sigmoid diverticulitis is vital for effective patient care. This comprehensive look will cover the location of the sigmoid colon, its typical anatomy, and how diverticulitis compares to other types of diverticular disease.
We’ll also delve into the pathophysiology, exploring the inflammatory process and potential complications.
This exploration will detail the physical changes in the sigmoid colon during an attack, discussing potential complications and long-term effects. The diagnostic methods used, from imaging techniques to symptom analysis, will be explored in depth. The common symptoms, potential variations, and the importance of recognizing atypical presentations will be highlighted. We will also review treatment options, from medical interventions to surgical procedures, providing a comparative analysis of advantages and disadvantages.
Finally, preventive strategies, lifestyle recommendations, and the significance of regular check-ups will be discussed.
Introduction to Sigmoid Diverticulitis
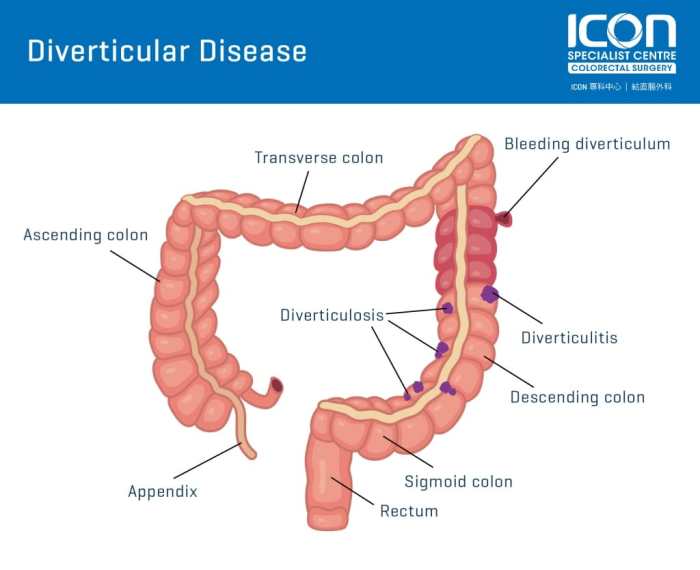
Sigmoid diverticulitis is a common inflammatory condition affecting the sigmoid colon, a crucial part of the large intestine. It involves the inflammation and infection of small pouches (diverticula) that protrude from the colon’s lining. Understanding the location and anatomy of the sigmoid colon, as well as the risk factors associated with this condition, is key to recognizing and managing it effectively.The sigmoid colon is the S-shaped portion of the large intestine that connects the descending colon to the rectum.
It’s located in the lower left quadrant of the abdomen, storing stool before it moves into the rectum for elimination. Its unique structure and function make it susceptible to specific issues.
Anatomy of the Sigmoid Colon
The sigmoid colon, characterized by its sigmoid (S-shaped) form, plays a critical role in the final stages of bowel preparation. It’s relatively mobile and has a thicker muscular layer compared to the other parts of the large intestine, adapting to the changes in stool consistency. This muscular layer helps to propel stool towards the rectum. The sigmoid colon’s lining is susceptible to developing diverticula, which are small, bulging pouches that can become inflamed.
Comparison of Diverticular Disease Types
| Feature | Sigmoid Diverticulitis | Diverticulosis | Other Types of Diverticular Disease (e.g., Diverticular Abscess, Fistula) |
|---|---|---|---|
| Location | Inflammation of diverticula primarily in the sigmoid colon | Presence of diverticula without inflammation | Inflammation or complications like abscesses or fistulas affecting diverticula, often in the sigmoid colon but can also be in other parts of the large intestine |
| Symptoms | Pain, fever, nausea, changes in bowel habits | Usually asymptomatic | Severe pain, fever, localized tenderness, potential for complications like sepsis |
| Treatment | Antibiotics, bowel rest, pain management | Usually no specific treatment required | May require surgical intervention, antibiotics, or other targeted therapies |
| Risk Factors | Similar to diverticulosis, but with potential for complications | Low-fiber diet, genetics, and aging | Often a complication of diverticulosis or sigmoid diverticulitis, or associated with other risk factors for inflammation |
Risk Factors for Sigmoid Diverticulitis, Sigmoid diverticulitis effect on the colon and diagnosis
A number of factors can increase a person’s likelihood of developing sigmoid diverticulitis. These include:
- Diet Low in Fiber: A diet lacking in fiber can lead to harder, drier stools, increasing pressure within the colon, and making it more prone to diverticula formation.
- Genetics: Family history of diverticular disease can increase the risk of developing the condition. Genetic predisposition plays a role in the structure and function of the colon, making some individuals more vulnerable.
- Age: The risk of diverticulitis generally increases with age, likely due to the natural aging process affecting the colon’s structure and function.
- Smoking: Smoking can negatively impact the health of the colon, increasing the risk of inflammation and other complications.
- Obesity: Being overweight or obese can increase the risk of developing diverticulitis due to factors such as increased pressure on the abdominal cavity and potential inflammatory responses.
Pathophysiology of Sigmoid Diverticulitis: Sigmoid Diverticulitis Effect On The Colon And Diagnosis
Sigmoid diverticulitis, a common inflammatory condition of the colon, primarily affects the sigmoid colon. Understanding its pathophysiology is crucial for accurate diagnosis and effective management. This involves comprehending the formation of diverticula, the inflammatory process, potential triggers, and how it differs from other inflammatory bowel diseases.
Diverticulum Formation
Diverticula are small, pouch-like herniations that protrude through the muscular layers of the colon wall. The exact mechanism of diverticulum formation isn’t fully understood, but it’s believed to be multifactorial. Increased intraluminal pressure, as seen with straining during bowel movements, and a weakened colonic wall due to factors like age, low fiber diet, and genetics are likely contributing factors.
A weakened bowel wall can make it more prone to bulging or herniation at points of weakness. This is a common finding in the sigmoid colon, the part of the large intestine where stool is collected before being eliminated.
Inflammation Process in Sigmoid Diverticulitis
Inflammation in sigmoid diverticulitis typically arises when fecal matter becomes trapped within the diverticula. This trapped material can lead to bacterial overgrowth and subsequent infection. The immune system responds to this infection, leading to an inflammatory cascade. Inflammation causes swelling, pain, and redness in the affected area. The inflammation can extend beyond the diverticula, potentially involving surrounding tissues and organs.
Possible Causes of Diverticulitis Inflammation
Several factors can contribute to the inflammatory response within the diverticula. Trapped fecal matter, as mentioned earlier, is a primary culprit. Additionally, the composition of the fecal matter itself can influence the risk. A diet low in fiber can lead to harder, drier stools, increasing intraluminal pressure and potentially causing irritation and inflammation. Bacterial overgrowth, a common occurrence in the colon, can also contribute to the inflammatory process.
A compromised immune system may also play a role in the development of inflammation.
Comparison with Other Inflammatory Bowel Diseases
While sigmoid diverticulitis involves inflammation in the colon, it differs from other inflammatory bowel diseases like Crohn’s disease and ulcerative colitis. Diverticulitis is characterized by inflammation confined primarily to the diverticula and surrounding tissue, often resolving with appropriate treatment. In contrast, Crohn’s disease and ulcerative colitis are chronic inflammatory conditions affecting the entire gastrointestinal tract, characterized by ongoing inflammation and potential complications.
The location, extent, and duration of inflammation distinguish diverticulitis from these other conditions.
Stages of Sigmoid Diverticulitis Progression
| Stage | Description | Symptoms | Management |
|---|---|---|---|
| Stage 1 (Acute Diverticulitis) | Mild inflammation limited to the diverticulum. | Mild abdominal pain, tenderness, fever, and altered bowel habits. | Conservative treatment (diet, antibiotics). |
| Stage 2 (Moderate Diverticulitis) | Inflammation extends beyond the diverticulum, potentially involving surrounding tissues. | Increased pain, fever, nausea, vomiting, and possible localized tenderness. | Antibiotics, possible hospitalization. |
| Stage 3 (Severe Diverticulitis) | Significant inflammation and potential complications such as abscess formation, perforation, or fistula development. | Severe abdominal pain, high fever, chills, septic shock, or signs of peritonitis. | Surgical intervention may be necessary. |
| Stage 4 (Complicated Diverticulitis) | Presence of severe complications like an abscess, perforation, or fistula, requiring urgent surgical intervention. | Symptoms escalate significantly, possibly including signs of sepsis. | Emergency surgical intervention (drainage, resection). |
Effects on the Colon
Sigmoid diverticulitis, a painful inflammatory condition, significantly impacts the sigmoid colon, the last section of the large intestine. Understanding the physical changes and potential complications is crucial for effective management and patient care. This section will detail the effects of diverticulitis on the colon, from the immediate inflammation to long-term consequences.
Physical Changes During a Diverticulitis Attack
Inflammation in the sigmoid colon during a diverticulitis attack is characterized by swelling and redness in the affected diverticula. The diverticula themselves, small pouches in the colon wall, can become inflamed and infected. The surrounding tissues also react, contributing to the overall inflammation and discomfort. This inflammation can cause the sigmoid colon to spasm, leading to pain and cramping.
Additionally, the affected area might experience increased pressure and tension, potentially compromising blood flow to the surrounding tissues.
Potential Complications
Sigmoid diverticulitis can lead to a range of complications, some of which can be serious. These complications often stem from the inflammatory process, which can extend beyond the immediate area and affect adjacent structures. The severity of complications varies greatly, depending on the individual and the extent of the diverticulitis.
Types of Complications
Several complications can arise from sigmoid diverticulitis. These include:
- Abscess Formation: A localized collection of pus can develop around the infected diverticula. This can cause significant pain and tenderness in the lower abdomen. Abscesses may require drainage, either through a surgical procedure or by a needle aspiration. For example, a patient experiencing persistent, severe abdominal pain along with fever might have an abscess requiring intervention.
- Fistula Formation: A fistula is an abnormal connection between the sigmoid colon and another organ, such as the bladder or vagina. This abnormal passageway can result in leakage of fecal material into other parts of the body, leading to further infections and complications. Fistulas require surgical repair to restore normal bodily functions. For example, a patient with recurring bowel infections and a history of diverticulitis may develop a fistula, requiring a more involved surgical procedure.
- Peritonitis: This serious complication occurs when the infection spreads from the diverticulitis to the lining of the abdominal cavity. Peritonitis is characterized by severe abdominal pain, fever, and signs of systemic illness. It necessitates immediate medical intervention, often including surgery to drain the infected fluid and address the underlying diverticulitis.
- Bowel Obstruction: The inflammation and scarring from diverticulitis can narrow or obstruct the sigmoid colon, preventing the passage of stool. This can lead to severe abdominal pain, nausea, vomiting, and a distended abdomen. In some cases, a surgical procedure is necessary to restore bowel function. For example, a patient with a history of recurrent diverticulitis and a sudden onset of severe abdominal pain and inability to pass stool might have a bowel obstruction requiring surgery.
Understanding the effects of sigmoid diverticulitis on the colon is crucial for diagnosis. Inflammation in the sigmoid colon can cause pain and discomfort, often requiring careful examination and testing. While this condition isn’t directly linked to types of heart disease , it’s important to note that some underlying health conditions might present with similar symptoms.
Ultimately, accurate diagnosis relies on a thorough assessment of the colon’s condition.
- Stricture Formation: Chronic inflammation can lead to the development of a stricture, a narrowing of the colon. This can impede the normal passage of stool, resulting in similar symptoms as bowel obstruction. The stricture may need to be dilated or surgically resected to restore normal bowel function.
Long-Term Effects
The long-term effects of sigmoid diverticulitis can range from minimal to significant, depending on the severity of the initial attack and the presence of complications. Chronic diverticulitis can lead to chronic pain, discomfort, and a reduced quality of life. In some cases, recurrent episodes of diverticulitis can necessitate more extensive surgical procedures. For example, repeated diverticulitis attacks could lead to the need for a colectomy (removal of part or all of the colon) in the future.
Potential Complications Table
| Complication | Description | Symptoms | Treatment |
|---|---|---|---|
| Abscess | Collection of pus | Severe abdominal pain, fever, tenderness | Drainage (surgical or needle aspiration) |
| Fistula | Abnormal connection to other organs | Leakage of fecal material, recurrent infections | Surgical repair |
| Peritonitis | Infection of abdominal lining | Severe abdominal pain, fever, signs of systemic illness | Immediate surgical intervention |
| Bowel Obstruction | Narrowing or blockage of the colon | Severe abdominal pain, nausea, vomiting, distended abdomen | Surgical intervention (possible bowel resection) |
| Stricture | Narrowing of the colon | Impacted stool, difficulty passing stool | Dilation or surgical resection |
Diagnostic Methods
Pinpointing the cause of sigmoid diverticulitis symptoms is crucial for effective treatment. Accurate diagnosis relies on a combination of patient history, physical examination, and various diagnostic tests. These methods help determine the extent of the inflammation, rule out other conditions, and guide treatment strategies.
Common Diagnostic Methods
Several methods are employed to diagnose sigmoid diverticulitis. These methods range from simple blood tests to more complex imaging techniques. Careful consideration of each method’s strengths and limitations is essential for accurate diagnosis.
Understanding the effects of sigmoid diverticulitis on the colon is key to proper diagnosis. Inflammation in the sigmoid colon can lead to pain and discomfort, and sometimes even complications. Before you buy Allegra, it’s crucial to remember that this medication is for allergies and won’t treat diverticulitis. Knowing the specific symptoms and getting a prompt diagnosis from a healthcare professional is essential for managing this condition effectively.
Ultimately, a thorough understanding of the condition and its effects on the colon is paramount.
- Patient History and Physical Examination: A detailed patient history, including symptoms (e.g., pain location, duration, bowel habits), medical history, and any recent dietary changes, is crucial. A physical examination, focusing on the abdomen, can help identify signs of inflammation, tenderness, or fever, which can suggest diverticulitis. However, these methods are not always definitive, and other conditions can present with similar symptoms.
- Blood Tests: Blood tests, such as a complete blood count (CBC) and inflammatory markers (e.g., C-reactive protein, erythrocyte sedimentation rate), can help assess inflammation. Elevated white blood cell count and inflammatory markers often indicate infection or inflammation, which can be present in sigmoid diverticulitis. However, these markers are not specific to diverticulitis and can be elevated in other conditions.
Imaging Techniques
Imaging plays a vital role in diagnosing sigmoid diverticulitis. It allows visualization of the affected area and helps distinguish diverticulitis from other conditions with similar symptoms.
- Abdominal X-rays: While not the primary imaging method for diverticulitis, abdominal X-rays can be useful to rule out other causes, such as bowel obstruction or free air. They can also show signs of a thickened bowel wall, but these signs are not specific to diverticulitis and may be present in other conditions. They are generally less informative than other imaging techniques for assessing diverticulitis.
- Computed Tomography (CT) Scan: A CT scan is the gold standard imaging technique for diagnosing sigmoid diverticulitis. It provides detailed cross-sectional images of the abdomen, allowing visualization of the colon and surrounding tissues. A CT scan can reveal the presence of diverticula, inflammation, abscess formation, or complications such as perforation. CT scans are highly accurate in identifying diverticulitis and its complications.
Examples of CT scan findings include thickened bowel wall, presence of diverticula, and pericolic fluid collections, characteristic of the inflammation.
- Ultrasound: Ultrasound is another imaging modality that can be used to assess the abdomen. It is particularly helpful in evaluating for fluid collections or abscesses. Ultrasound is often less sensitive than CT scans in detecting diverticulitis, especially in cases with less significant inflammation. It can be a good initial assessment tool, especially if CT scans are not readily available.
- Magnetic Resonance Imaging (MRI): MRI can also be used to visualize the colon and surrounding tissues. While MRI is excellent for soft tissue imaging, it is generally less frequently used for initial diagnosis of diverticulitis compared to CT scans due to longer scanning times and potential cost concerns. However, it can provide valuable information in specific cases where certain features might be better visualized by MRI than by CT scan.
Comparison of Imaging Modalities
| Imaging Modality | Accuracy | Limitations | Usefulness in Diverticulitis |
|---|---|---|---|
| Abdominal X-ray | Moderate | Less detailed visualization, not specific for diverticulitis | Useful for ruling out other conditions but not ideal for diagnosis |
| CT Scan | High | Exposure to radiation, potential for contrast allergies | Gold standard for diagnosing diverticulitis and complications |
| Ultrasound | Moderate | Limited visualization of deeper structures, operator dependence | Useful for evaluating for fluid collections but not as detailed as CT |
| MRI | High | Longer scanning times, potentially higher cost | Can be helpful in specific cases, not the primary choice for initial diagnosis |
Symptoms and Signs
Understanding the symptoms of sigmoid diverticulitis is crucial for early diagnosis and effective management. The presentation can vary significantly, and recognizing atypical symptoms is essential for prompt intervention. This can significantly impact the patient’s recovery and overall health outcomes. Early detection often leads to better treatment results.
Common Symptoms of Sigmoid Diverticulitis
The symptoms of sigmoid diverticulitis are often subtle initially, and their severity can range from mild discomfort to severe abdominal pain. A thorough understanding of the typical and atypical presentations can aid in timely diagnosis and appropriate treatment. Patients should be encouraged to report any unusual or persistent symptoms to their healthcare provider.
Variations in Symptom Presentation
The presentation of sigmoid diverticulitis symptoms can vary widely, depending on the severity and location of the inflammation. Some individuals may experience only mild, intermittent discomfort, while others may present with severe, acute pain. The presence of fever, nausea, or vomiting can also vary significantly. The location of the pain may be localized to the lower left quadrant of the abdomen, or it might radiate to other areas.
Understanding sigmoid diverticulitis involves knowing how it affects the colon and the diagnostic process. Sometimes, similar pain can be mistaken for issues like injuries and conditions causing hip pain, which can be tricky to distinguish. For example, severe pain radiating from the lower abdomen to the hip region can be a symptom of diverticulitis, mimicking the discomfort of injuries and conditions causing hip pain.
Ultimately, accurate diagnosis requires a thorough examination and consideration of other potential factors impacting the colon.
Importance of Recognizing Atypical Presentations
Recognizing atypical presentations of sigmoid diverticulitis is critical for timely diagnosis and treatment. Certain individuals may not exhibit the classic symptoms, such as lower left quadrant pain. These atypical presentations might include symptoms such as fatigue, generalized abdominal discomfort, or subtle changes in bowel habits. Atypical presentations can delay diagnosis if healthcare providers are not aware of the potential variations.
Potential Symptoms with Severity Levels
Patients experiencing sigmoid diverticulitis may exhibit a range of symptoms, varying in severity. It is crucial for healthcare providers to carefully evaluate the patient’s reported symptoms, considering the severity of each. This evaluation can assist in establishing an accurate diagnosis and determining the appropriate treatment approach.
Typical Symptoms and Severity in Sigmoid Diverticulitis
| Symptom | Mild | Moderate | Severe |
|---|---|---|---|
| Abdominal Pain (LLQ) | Localized, mild ache | Moderate, persistent pain | Intense, sharp, constant pain |
| Fever | Absent or low-grade | Moderate fever (101-102°F) | High fever (103°F or higher) |
| Nausea/Vomiting | Absent | Occasional nausea or vomiting | Frequent nausea and vomiting |
| Changes in Bowel Habits | Occasional diarrhea or constipation | More frequent diarrhea or constipation | Severe diarrhea, inability to pass stool |
| Tenderness | Mild tenderness to touch | Moderate tenderness to the touch | Severe tenderness, guarding |
Treatment Options
Sigmoid diverticulitis, a common inflammatory condition of the colon, necessitates a tailored treatment approach based on the severity of the inflammation and the patient’s overall health. Effective management aims to alleviate symptoms, prevent complications, and promote healing. The treatment strategy often involves a combination of medical and, in some cases, surgical interventions.The goal of treatment for sigmoid diverticulitis is multifaceted, encompassing pain relief, resolution of inflammation, prevention of recurrence, and identification and management of any potential complications.
Different treatment strategies are employed depending on the individual patient’s presentation, including the extent of the inflammation, the presence of complications, and the patient’s overall health.
Common Treatment Approaches
Treatment options for sigmoid diverticulitis generally fall into two categories: medical management and surgical intervention. Medical management is the first line of defense, often sufficient for uncomplicated cases. Surgical intervention is reserved for cases with complications, severe disease, or those who do not respond to medical therapy.
Medical Interventions
Medical management typically involves a combination of strategies aimed at reducing inflammation, managing pain, and preventing complications. These strategies include:
- Resting the Bowels: A crucial aspect of medical management involves a low-fiber diet to minimize bowel stimulation and allow the inflamed area to heal. This dietary restriction, often recommended for several days to a week, is often paired with hydration to avoid dehydration. Specific instructions regarding the duration and composition of the diet are tailored to each patient’s needs.
- Antibiotics: Antibiotics are commonly prescribed to address the infection associated with sigmoid diverticulitis. These medications target the bacteria that contribute to the inflammation and infection, helping to reduce the inflammatory response. The specific type and duration of antibiotic therapy are determined by the severity of the infection and the patient’s response to treatment. Broad-spectrum antibiotics are often used initially, followed by a more targeted approach if necessary.
Examples of antibiotics include metronidazole, ciprofloxacin, or a combination of both.
- Analgesics: Over-the-counter pain relievers, such as ibuprofen or naproxen, are often effective in managing the pain associated with diverticulitis. In more severe cases, stronger opioid pain medications may be necessary, though their use is often limited to a short-term basis. Pain management strategies are individualized and tailored to the intensity of the pain experienced by the patient.
Surgical Treatment Options
Surgical interventions are typically reserved for patients with complicated cases of sigmoid diverticulitis, such as abscess formation, fistula development, or perforation. Procedures may include:
- Drainage of Abscesses: Surgical drainage of abscesses is performed to remove the collection of pus and infected material. This procedure is often performed using minimally invasive techniques, such as percutaneous drainage, or through an incision to ensure complete drainage of the infected area.
- Fistula Repair: A fistula is an abnormal connection between two organs. Surgical repair of a fistula associated with sigmoid diverticulitis aims to restore normal organ function and prevent recurrence of the fistula.
- Colectomy: In severe cases, a colectomy, the surgical removal of a portion of the colon, may be necessary. This procedure is typically reserved for cases with recurrent diverticulitis, severe complications, or when other treatment options have failed. The extent of the colectomy varies depending on the severity and location of the diverticulitis.
Comparison of Treatment Options
| Treatment Option | Advantages | Disadvantages | Considerations |
|---|---|---|---|
| Medical Management | Non-invasive, less costly, often effective for uncomplicated cases | May not be effective for complicated cases, potential for recurrence | Severity of infection, patient response to treatment |
| Surgical Intervention | Effective for complicated cases, potentially curative | More invasive, higher risk of complications (e.g., infection, bleeding), longer recovery time | Presence of abscesses, fistulas, perforation |
Prevention and Management
Sigmoid diverticulitis, while often manageable, can be a recurring issue. Proactive steps, focusing on lifestyle choices and regular medical attention, can significantly reduce the risk of developing the condition or experiencing future flare-ups. This section delves into strategies for preventing sigmoid diverticulitis and managing the condition effectively.A healthy lifestyle forms the cornerstone of preventing diverticulitis. Maintaining a balanced diet and regular exercise plays a crucial role in overall health and can lessen the likelihood of developing diverticula and related complications.
This holistic approach emphasizes the interconnectedness of diet, activity, and preventative healthcare.
Dietary Recommendations
A diet rich in fiber is essential for promoting digestive health and potentially reducing the risk of diverticulitis. Fiber helps regulate bowel movements, making them softer and easier to pass, thereby reducing strain on the colon. Dietary modifications can significantly influence the risk of diverticulitis.
- Increasing fiber intake gradually is crucial. A sudden increase can lead to digestive discomfort. Start by incorporating high-fiber foods like fruits, vegetables, and whole grains into your diet, gradually increasing the amount over time. This allows the digestive system to adjust to the higher fiber content.
- Hydration is equally important. Adequate water intake aids in maintaining the softness of stools, making them easier to pass and reducing the risk of constipation, a known risk factor for diverticulitis.
- Limiting processed foods, red meat, and excessive saturated fats can contribute to overall digestive health. These foods are often lower in fiber and may potentially exacerbate existing diverticulitis symptoms or increase the risk of developing it.
Lifestyle Strategies
Maintaining a healthy weight and regular physical activity are vital for overall well-being and can influence the risk of developing diverticulitis. Regular exercise helps maintain a healthy weight, supports bowel regularity, and strengthens the body’s overall resilience.
- Maintaining a healthy weight can reduce pressure on the colon, potentially decreasing the risk of diverticula formation.
- Regular physical activity promotes healthy bowel movements and strengthens the body’s overall function, improving its ability to handle digestive processes.
- Stress management techniques, such as meditation, yoga, or deep breathing exercises, can also play a role in overall well-being and digestive health.
Importance of Regular Check-ups
Regular check-ups and screenings are vital for early detection and management of diverticulitis. These appointments allow healthcare professionals to monitor overall health, assess risk factors, and provide timely intervention if needed. Early detection and prompt treatment can prevent complications and reduce the severity of the condition.
- Regular colonoscopies, when recommended by a healthcare professional, can detect diverticula and other potential issues in the colon early, enabling timely intervention and potentially preventing complications.
- Regular check-ups also allow healthcare providers to monitor any changes in symptoms, adjust treatment plans, and address potential underlying conditions that might contribute to diverticulitis.
- Following the advice of healthcare professionals regarding screenings and preventive measures is crucial. This personalized approach ensures tailored recommendations based on individual health history and risk factors.
Preventive Measures and Effectiveness
While definitive prevention of diverticulitis isn’t always possible, implementing the strategies mentioned can significantly reduce the risk. Studies have shown a correlation between high-fiber diets and a lower incidence of diverticulitis.
- Examples of preventive measures include: adopting a high-fiber diet, maintaining a healthy weight, engaging in regular physical activity, and managing stress effectively. These measures are proven effective when consistently implemented and combined with proper medical care.
Final Review
In conclusion, sigmoid diverticulitis, affecting the sigmoid colon, presents a range of complexities in terms of diagnosis and treatment. Understanding the diverse factors, from pathophysiology to potential complications, is essential for optimal patient care. This comprehensive overview provides a solid foundation for comprehending the intricacies of this condition, from the initial stages to long-term management. Early diagnosis and prompt treatment are key to mitigating potential complications and ensuring a positive patient outcome.




