COVID causes new high blood pressure, a concerning link that’s emerging as a significant public health concern. High blood pressure, a prevalent condition, has always been a major health issue. Now, the potential for COVID-19 to exacerbate or even initiate this problem demands closer investigation. The potential mechanisms are multifaceted, ranging from inflammatory responses to blood clots, with pre-existing conditions and the severity of infection playing significant roles.
Understanding these intricate relationships is crucial for developing effective preventative and treatment strategies.
This article delves into the potential connections between COVID-19 and elevated blood pressure. We’ll explore the underlying mechanisms, risk factors, diagnostic considerations, treatment strategies, and the ongoing research efforts to fully understand this complex relationship. A comprehensive look at the potential impact on vulnerable populations is also crucial to understanding the full picture.
The COVID-19 Connection to High Blood Pressure
High blood pressure, or hypertension, is a significant global health concern, affecting millions worldwide. It’s a leading risk factor for heart disease and stroke, and its prevalence has been steadily increasing. The COVID-19 pandemic has introduced a new layer of complexity to this issue, with emerging evidence suggesting a potential link between infection and elevated blood pressure. This article explores this relationship, delving into the historical context of hypertension, the possible mechanisms by which COVID-19 might contribute to high blood pressure, and the factors influencing this connection.
Historical Context of High Blood Pressure
High blood pressure has been recognized as a serious health issue for decades. Early studies established its strong correlation with cardiovascular events. The increasing prevalence of hypertension over time underscores the critical need for prevention and management strategies. This growing burden has prompted extensive research into its causes, risk factors, and effective treatments. The ongoing effort to understand and combat hypertension is crucial to public health.
Potential Mechanisms of COVID-19’s Impact on Blood Pressure
COVID-19’s impact on blood pressure is a complex phenomenon with multiple potential mechanisms. The inflammatory response triggered by the virus can directly affect blood vessels, leading to increased stiffness and constriction. Furthermore, the virus’s impact on the renin-angiotensin-aldosterone system (RAAS) can also contribute to elevated blood pressure. The disruption of this vital system regulates blood volume and pressure.
The cytokine storm, a characteristic overreaction of the immune system, may further contribute to the elevated blood pressure.
Factors Influencing the COVID-19-Hypertension Relationship
Several factors can influence the link between COVID-19 and high blood pressure. Pre-existing conditions, such as obesity, diabetes, and a family history of hypertension, can significantly increase susceptibility. The severity of COVID-19 infection itself plays a role; more severe cases may be associated with more pronounced blood pressure changes. Other factors such as age and ethnicity may also contribute to the variations in this relationship.
Summary Table: Factors Influencing the Relationship
| Factor | Potential Impact on Blood Pressure | Evidence |
|---|---|---|
| Pre-existing conditions (e.g., obesity, diabetes) | Increased susceptibility to elevated blood pressure following COVID-19 infection. | Studies show that individuals with pre-existing conditions often experience more severe outcomes. |
| Severity of COVID-19 infection | More severe cases may be associated with more pronounced blood pressure changes. | Hospitalized patients with severe COVID-19 often exhibit elevated blood pressure. |
| Age | Older individuals may be more susceptible to blood pressure increases following COVID-19 infection. | Studies have shown a correlation between age and the severity of COVID-19 and associated complications. |
| Ethnicity | Certain ethnic groups may experience varying degrees of blood pressure response to COVID-19 infection. | Studies exploring the racial disparities in COVID-19 outcomes might shed light on this aspect. |
COVID-19 and Blood Pressure
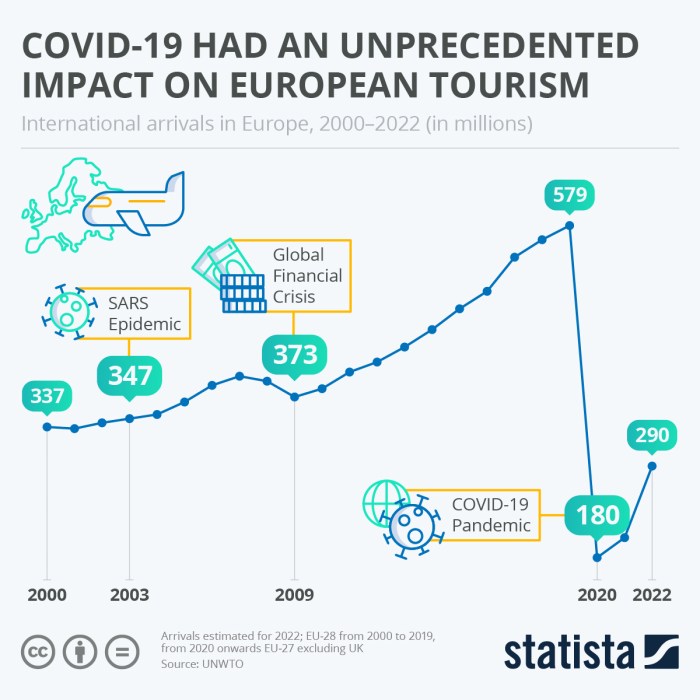
The link between COVID-19 and high blood pressure is a growing concern for researchers and healthcare professionals. While the exact mechanisms are still under investigation, several potential pathways are being explored. Understanding these mechanisms is crucial for developing targeted interventions and preventative strategies.
Potential Inflammatory Pathways
Inflammation plays a significant role in the development and progression of high blood pressure. COVID-19 infection can trigger a complex inflammatory response within the body, potentially affecting blood vessels and contributing to hypertension. Cytokines, signaling molecules that regulate inflammation, are released in response to the virus. These molecules can induce vascular dysfunction and contribute to the narrowing of blood vessels.
This narrowing increases resistance to blood flow, leading to higher blood pressure.
Role of the Immune System Response
The immune system’s response to COVID-19 infection can also contribute to the development of hypertension. The body’s immune cells, like T cells and macrophages, play a critical role in fighting the virus. However, an overactive or prolonged immune response can lead to chronic inflammation, contributing to vascular damage and high blood pressure.
Blood Clots and Hypertension
Blood clots are a serious complication of COVID-19. While the exact relationship between blood clots and hypertension isn’t fully understood, a possible connection exists. Inflammation caused by the virus can increase the risk of blood clots forming, and these clots can affect blood flow, contributing to high blood pressure. Furthermore, the body’s response to the clots can further exacerbate inflammation, creating a cycle that contributes to hypertension.
Recent studies highlight a surprising link between COVID and high blood pressure. While the exact mechanisms are still being researched, the impact on cardiovascular health is undeniable. Interestingly, this new understanding of the health impacts of COVID might lead to further questions about how other conditions, like Irritable Bowel Syndrome (IBS) diarrhea, affect medications like birth control pills.
For more information on this topic, check out this helpful article on does ibs diarrhea affect birth control pills. Ultimately, the long-term effects of COVID on our health are still a major area of investigation.
Impact of Viral Load on Blood Pressure Regulation
Viral load, the amount of virus present in the body, can significantly impact blood pressure regulation. Higher viral loads may trigger a stronger inflammatory response, potentially leading to more pronounced increases in blood pressure. This can vary among individuals based on factors such as age, pre-existing health conditions, and the specific strain of the virus.
Comparison of Inflammatory Responses
| Characteristic | Individuals with High Blood Pressure | Individuals without High Blood Pressure |
|---|---|---|
| Cytokine Release | Higher initial cytokine release, prolonged elevation. | Modest and more transient cytokine release. |
| Vascular Reactivity | Increased sensitivity to vasoconstrictors. | Lower sensitivity to vasoconstrictors. |
| Inflammation Markers | Higher levels of inflammatory markers in blood. | Lower levels of inflammatory markers in blood. |
| Blood Vessel Function | Reduced endothelial function, increased oxidative stress. | Preserved endothelial function, lower oxidative stress. |
| Immune System Response | Potentially more exaggerated or sustained immune response. | More controlled and balanced immune response. |
This table highlights potential differences in inflammatory responses between individuals with and without pre-existing high blood pressure. The individuals with high blood pressure often exhibit a more pronounced and prolonged inflammatory response, which may contribute to the development or worsening of hypertension. Further research is needed to confirm these observations.
Risk Factors and Population Impacts
The lingering effects of COVID-19 extend beyond the initial illness, impacting various aspects of health, including cardiovascular function. Emerging research suggests a correlation between COVID-19 infection and an increased risk of developing or exacerbating high blood pressure. Understanding the factors contributing to this link, and the populations most vulnerable, is crucial for effective preventative measures and targeted interventions.This section delves into the risk factors associated with post-COVID-19 hypertension, highlighting vulnerable populations and potential long-term consequences.
It also examines the prevalence of high blood pressure in individuals with a history of COVID-19 compared to those without.
Risk Factors Increasing Post-COVID Hypertension
Several factors can elevate the risk of developing high blood pressure following a COVID-19 infection. These factors may interact in complex ways, potentially leading to heightened susceptibility in certain individuals.
- Severity of COVID-19 infection: Individuals who experienced severe COVID-19 symptoms, including pneumonia or intensive care unit (ICU) admission, may face a higher risk of developing hypertension post-infection. The inflammatory response associated with severe illness can potentially damage blood vessel linings, leading to increased blood pressure.
- Pre-existing conditions: Individuals with pre-existing cardiovascular risk factors, such as obesity, diabetes, or a family history of hypertension, may be more susceptible to developing or worsening high blood pressure after COVID-19. These pre-existing conditions can exacerbate the inflammatory response associated with the infection.
- Age: Older adults, often with underlying health conditions, tend to be at a higher risk for developing complications like hypertension after a COVID-19 infection. The aging process itself can impact blood pressure regulation, and the inflammatory response to COVID-19 can further exacerbate these changes.
- Inflammation: The inflammatory response triggered by the COVID-19 virus can directly affect blood vessels, potentially leading to sustained increases in blood pressure. This inflammatory response can be prolonged even after the acute infection resolves.
Vulnerable Populations
Certain populations are disproportionately affected by the correlation between COVID-19 and hypertension. Recognizing these vulnerabilities is essential for tailored interventions.
Recent studies show COVID can unfortunately lead to a spike in high blood pressure cases. Managing this new health challenge often involves lifestyle changes, like choosing the right cooking oils. For example, incorporating healthier options like olive oil or avocado oil into your diet, as detailed in this helpful guide on healthiest cooking oils for high cholesterol , can be a crucial step in maintaining heart health.
This, in turn, can positively impact blood pressure management for those dealing with COVID-related high blood pressure.
- Individuals with pre-existing cardiovascular conditions: Those with a history of heart disease, high cholesterol, or diabetes are at increased risk for post-COVID-19 hypertension. The underlying conditions can interact with the effects of the virus to increase the risk.
- Obese individuals: Obesity is a significant risk factor for hypertension. The combination of obesity and COVID-19 infection may further increase the likelihood of developing or exacerbating high blood pressure due to increased inflammation and vascular dysfunction.
- Older adults: As mentioned previously, older adults are often more susceptible to complications due to their underlying health conditions and the impact of aging on blood pressure regulation.
- Ethnic minorities: Certain ethnic groups may experience higher rates of COVID-19 severity and longer-term complications, potentially contributing to a disproportionate impact on hypertension rates.
Prevalence Comparison
Studies comparing the prevalence of high blood pressure in individuals with a history of COVID-19 versus those without are ongoing. Early findings suggest a potential increase in hypertension among those who have had the infection. Further research is needed to establish definitive prevalence rates and identify specific factors contributing to this correlation.
Long-Term Effects on Blood Pressure Regulation, Covid causes new high blood pressure
The long-term effects of COVID-19 on blood pressure regulation are an area of active research. Potential mechanisms include persistent inflammation, vascular damage, and altered autonomic nervous system function. Understanding these mechanisms is crucial for developing preventative and therapeutic strategies.
Risk Factors, Impact, and Evidence Table
| Risk Factor | Potential Impact | Supporting Evidence |
|---|---|---|
| Severity of COVID-19 infection | Increased risk of post-infection hypertension due to prolonged inflammation and vascular damage. | Observational studies and clinical trials showing a correlation between severe COVID-19 and subsequent hypertension. |
| Pre-existing cardiovascular conditions | Individuals with pre-existing conditions may experience a more pronounced increase in blood pressure after infection. | Existing literature on the interaction of pre-existing conditions and infections in increasing hypertension risk. |
| Age | Older adults often exhibit a higher risk of developing hypertension after COVID-19 due to underlying health conditions and age-related changes in blood pressure regulation. | Studies demonstrating the increased vulnerability of older adults to various health complications after infection. |
| Obesity | Obesity can exacerbate the inflammatory response and vascular dysfunction associated with COVID-19, increasing hypertension risk. | Research linking obesity to increased inflammation and blood pressure. |
Diagnostic Considerations
Post-COVID-19, maintaining vigilance regarding blood pressure is crucial. While the exact mechanisms linking COVID-19 and hypertension are still under investigation, a significant number of individuals experience elevated blood pressure after infection. This necessitates a proactive approach to diagnosis and management. Understanding the diagnostic considerations can help individuals and healthcare providers take the necessary steps to prevent long-term health complications.
Importance of Regular Blood Pressure Monitoring
Regular blood pressure monitoring is paramount for individuals who have had COVID-19. This proactive approach allows for early detection of any elevated blood pressure, enabling timely intervention and management. Prolonged high blood pressure can lead to severe health problems, including cardiovascular disease and stroke. Consistent monitoring allows healthcare providers to track trends and adjust treatment plans as needed.
This practice significantly contributes to better health outcomes and reduces the risk of serious complications.
Recommended Diagnostic Procedures
Standard blood pressure measurement techniques are employed to evaluate blood pressure. A trained healthcare professional typically takes several readings using a calibrated sphygmomanometer and stethoscope, or an automated blood pressure monitor. These measurements are taken at various points during the day to capture fluctuations and to obtain a comprehensive understanding of the individual’s blood pressure profile. A detailed medical history is crucial in providing context for the blood pressure readings.
Key Questions for Healthcare Providers
During patient assessments, healthcare providers should inquire about the patient’s medical history, including prior hypertension diagnoses, family history of hypertension, and current medications. Additionally, they should ascertain the severity and duration of the COVID-19 infection. The presence of any associated symptoms, such as headaches, dizziness, or chest pain, should also be explored. Gathering this information helps healthcare professionals in assessing the patient’s individual risk factors and tailoring the diagnostic approach accordingly.
Diagnostic Criteria for High Blood Pressure and Potential Complications
| Diagnostic Criteria | Potential Complications |
|---|---|
| Systolic blood pressure consistently above 140 mmHg or diastolic blood pressure consistently above 90 mmHg | Increased risk of cardiovascular disease, stroke, kidney damage, and other serious health problems. |
| Elevated blood pressure readings after COVID-19 infection, especially if accompanied by other risk factors | Potential for the development of chronic hypertension, requiring ongoing management and monitoring. |
| Presence of pre-existing hypertension conditions | Increased risk of exacerbating existing conditions and the potential for developing further complications after COVID-19 infection. |
| Age, gender, and family history of hypertension | Contributing factors to the overall risk profile and potential development of high blood pressure. |
Consistent monitoring and proactive management are crucial in mitigating the potential risks of elevated blood pressure following a COVID-19 infection.
Treatment and Management Strategies
Post-COVID-19 high blood pressure presents a unique challenge, requiring a multifaceted approach that goes beyond standard hypertension management. Effective strategies must address both the immediate needs of the individual and the potential for long-term complications. Lifestyle modifications play a crucial role in mitigating risk, while appropriate medication, if needed, can help control blood pressure.Comprehensive management hinges on a patient-centered approach, recognizing the individual’s specific circumstances and needs.
The long-term monitoring and support provided by healthcare professionals are critical for sustained health outcomes. By combining lifestyle adjustments, potential medication, and ongoing support, individuals can work toward better control and minimize the risk of long-term health problems.
Lifestyle Modifications
Lifestyle modifications are foundational in managing hypertension, regardless of its cause. For those with post-COVID-19 hypertension, these modifications are particularly important for reducing blood pressure and improving overall health. A balanced diet, regular exercise, and stress management are key components of an effective strategy.
- Dietary Changes: A diet rich in fruits, vegetables, and whole grains, with a reduced intake of sodium, saturated fats, and processed foods, can significantly impact blood pressure. Reducing excessive alcohol consumption is also crucial. Examples include incorporating more potassium-rich foods, such as bananas and spinach, and limiting intake of foods high in sodium, such as processed meats and fast food.
- Regular Exercise: Aerobic exercise, such as brisk walking, jogging, or swimming, helps lower blood pressure and improve cardiovascular health. Consistent, moderate-intensity exercise, for example, 30 minutes most days of the week, is highly beneficial. Strength training can also contribute to overall well-being and improve blood pressure control.
- Stress Management: Chronic stress can exacerbate high blood pressure. Techniques such as meditation, yoga, and deep breathing exercises can help manage stress levels and contribute to better blood pressure control. Prioritizing sleep and establishing a regular sleep schedule can also significantly impact stress levels.
Medication for Hypertension
The potential role of medication in managing hypertension after COVID-19 depends on the severity and persistence of elevated blood pressure. In cases where lifestyle modifications are insufficient, or if blood pressure remains consistently high, medication may be necessary. The choice of medication will be individualized, considering the patient’s overall health and other conditions.
- Selection of Medications: Commonly prescribed antihypertensive medications include diuretics, beta-blockers, ACE inhibitors, and calcium channel blockers. Each medication class has potential benefits and risks, which will be discussed in the table below. The healthcare provider will carefully consider the patient’s individual circumstances when selecting the most appropriate medication.
Long-Term Monitoring and Support
Long-term monitoring and support are essential for individuals with post-COVID-19 hypertension. Regular blood pressure checks, adherence to treatment plans, and ongoing communication with healthcare providers are crucial for maintaining optimal blood pressure control. This monitoring ensures that any necessary adjustments to medication or lifestyle can be made promptly, and it allows for early detection of potential complications.
- Regular Check-ups: Regular appointments with a healthcare provider are necessary for monitoring blood pressure, assessing overall health, and adjusting treatment plans as needed. This allows for proactive management of blood pressure and potential complications. For instance, a patient might need more frequent visits in the first year after diagnosis to ensure blood pressure remains stable.
- Patient Education: Educating patients about their condition, treatment plan, and potential complications is vital. This empowers them to take an active role in their health management and improves adherence to treatment recommendations.
Treatment Options Table
| Treatment Option | Potential Benefits | Potential Risks |
|---|---|---|
| Diuretics | Effective in lowering blood pressure, readily available, and generally well-tolerated. | Potential for dehydration, electrolyte imbalances, and increased risk of other medical complications, depending on the individual. |
| Beta-blockers | Effective in lowering blood pressure and reducing heart rate, particularly useful in cases of high blood pressure with accompanying heart conditions. | Potential side effects such as fatigue, dizziness, and slowed heart rate. Not suitable for all individuals, especially those with respiratory conditions. |
| ACE Inhibitors | Effective in lowering blood pressure and potentially beneficial for kidney health. | Potential side effects including cough, dizziness, and kidney problems. Not recommended for pregnant women. |
| Calcium Channel Blockers | Effective in lowering blood pressure, and generally well-tolerated, suitable for individuals with other conditions. | Potential side effects such as headache, swelling in the ankles, and dizziness. |
Research and Future Directions
The connection between COVID-19 and high blood pressure is a complex and rapidly evolving area of research. While initial studies have shown a correlation, understanding the precise mechanisms driving this link is crucial for developing effective preventive and therapeutic strategies. Further research is essential to fully grasp the intricate relationship and tailor interventions for at-risk populations.
Current Research Efforts
Numerous studies are currently underway to unravel the complex interplay between COVID-19 and high blood pressure. Researchers are employing various methodologies, including epidemiological studies analyzing large patient cohorts, to identify patterns and risk factors. These investigations are focusing on specific factors such as the severity of COVID-19 infection, pre-existing blood pressure conditions, and the use of specific medications.
These studies aim to establish a causal link between the virus and the elevated blood pressure readings observed in some patients.
Identifying Specific Mechanisms
Pinpointing the exact mechanisms by which COVID-19 might influence blood pressure regulation remains a key challenge. Researchers are investigating potential inflammatory pathways, the impact of the virus on the cardiovascular system, and the role of specific viral proteins. Understanding these intricate mechanisms will pave the way for targeted interventions, leading to more effective treatment strategies. The intricate interplay between the immune response to the virus and the cardiovascular system is being explored to determine the specific mechanisms driving the observed blood pressure changes.
Developing New Therapeutic Approaches
The potential for developing new therapeutic approaches to address the COVID-19-related high blood pressure issue is substantial. This includes the development of novel drugs targeting the inflammatory pathways activated by the virus or the cardiovascular mechanisms implicated in the blood pressure increase. Furthermore, the exploration of existing medications with potential anti-inflammatory or cardiovascular benefits in this context is also an active area of research.
Clinical trials are necessary to assess the safety and efficacy of these potential treatments. This could involve repurposing existing drugs with anti-inflammatory properties, or investigating novel targets within the body’s inflammatory response.
Key Areas Needing Further Investigation and Research Gaps
| Area of Investigation | Research Gap |
|---|---|
| Long-term effects on blood pressure | Understanding the persistence of elevated blood pressure readings after COVID-19 infection is crucial for developing appropriate long-term management strategies. |
| Role of specific viral proteins | Identifying the specific viral proteins involved in triggering cardiovascular responses and high blood pressure is essential to develop targeted therapies. |
| Impact of pre-existing conditions | Determining how pre-existing conditions, such as diabetes or obesity, influence the severity of blood pressure elevation after COVID-19 infection is critical for risk stratification. |
| Effectiveness of existing medications | Investigating the effectiveness of existing anti-inflammatory or cardiovascular medications in mitigating blood pressure elevation in COVID-19 patients is a priority. |
| Specific genetic predispositions | Identifying genetic factors that may increase susceptibility to blood pressure elevation after COVID-19 infection will help target high-risk individuals. |
Public Health Implications
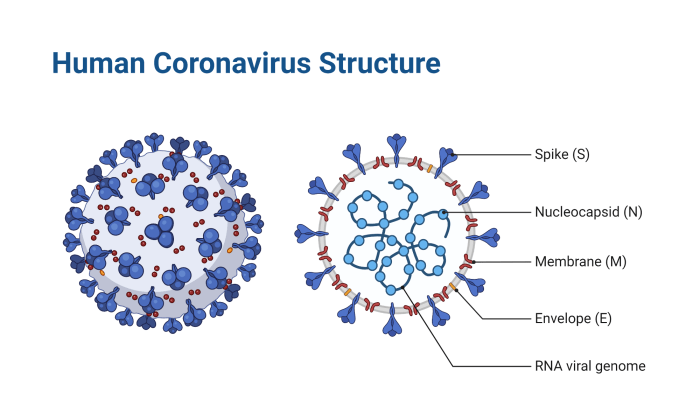
The surge in COVID-19-related high blood pressure presents a significant public health concern. The long-term implications for individuals and the strain on healthcare systems are substantial, necessitating proactive strategies to mitigate the impact. Understanding these implications is crucial for developing effective preventative measures and resource allocation plans.
Potential Burden on Healthcare Systems
The rise in hypertension, potentially linked to COVID-19, will inevitably strain healthcare resources. Increased hospital admissions, longer stays, and higher demands on specialized medical personnel will be unavoidable consequences. This pressure extends beyond direct medical care, affecting diagnostic tools, medication supply, and the overall efficiency of the healthcare system.
Impact on Resource Allocation
Addressing this emerging health challenge necessitates careful resource allocation. Funding for research, preventative care programs, and expanded healthcare capacity will be critical. Prioritizing high-risk populations, such as the elderly and those with pre-existing conditions, is essential to minimize the health disparities that may arise.
Public Awareness Campaigns and Preventive Measures
Public awareness campaigns are paramount to promoting lifestyle modifications that can reduce the risk of COVID-19-induced hypertension. Educational programs focusing on healthy diets, regular exercise, stress management, and the importance of early detection of blood pressure issues will be crucial. Collaboration between healthcare providers, community organizations, and public health agencies is essential for effective dissemination of information and program implementation.
| Category | Potential Impact | Example |
|---|---|---|
| Hospitalizations | Increased number of patients requiring hospitalization for hypertension-related complications. | A surge in patients needing intensive care units (ICUs) for hypertension crises. |
| Emergency Room Visits | Higher frequency of emergency room visits for blood pressure management. | A 15% increase in emergency room visits for hypertension in a specific region over a year. |
| Medication Supply | Increased demand for antihypertensive medications, potentially leading to shortages. | A 20% increase in prescriptions for blood pressure medication in the first quarter of the year. |
| Healthcare Personnel | Strain on healthcare providers to manage the growing number of hypertension cases. | Increased workload and burnout among nurses and doctors in hospitals dealing with COVID-19 related hypertension. |
“A robust public health response is crucial to manage the potential burden of COVID-19-associated hypertension on healthcare systems.”
Recommendations for Prevention
Implementing preventive measures is vital to mitigating the future impact of this public health concern. These measures include:
- Promoting healthy lifestyle choices, including balanced diets, regular physical activity, and stress reduction techniques.
- Encouraging regular blood pressure screenings, particularly in vulnerable populations.
- Strengthening community-based health initiatives to facilitate access to care and education.
Outcome Summary: Covid Causes New High Blood Pressure
In conclusion, the connection between COVID-19 and new-onset high blood pressure is a complex issue demanding further investigation. While research is ongoing, the potential impact on public health is substantial. From understanding the inflammatory pathways triggered by the virus to identifying vulnerable populations, regular monitoring and proactive measures are key. This article has presented a comprehensive overview, providing insights into the mechanisms, risk factors, and potential solutions.
Further research is vital to unravel the intricacies of this link and ultimately mitigate its negative health consequences.




