Are severe sleep apnea and CPAP pressure correlated? This question delves into the intricate relationship between the severity of sleep apnea and the optimal CPAP pressure needed for effective treatment. Understanding this correlation is crucial for personalized CPAP therapy, optimizing patient outcomes, and potentially revolutionizing sleep apnea management. We’ll explore various aspects, from the different types of sleep apnea and their characteristics to the methods used to assess severity and the factors influencing the correlation.
This investigation will cover the fundamental concepts of sleep apnea and CPAP, examining the different pressure settings and their impact on the respiratory system. We’ll then delve into how sleep apnea severity is measured, focusing on the crucial role of the apnea-hypopnea index (AHI). A key part of the discussion will be the relationship between AHI and optimal CPAP pressure, providing a clear understanding of the connection between these two critical factors.
Introduction to Sleep Apnea and CPAP Pressure: Are Severe Sleep Apnea And Cpap Pressure Correlated
Sleep apnea is a common sleep disorder characterized by pauses in breathing during sleep. These pauses can last from a few seconds to a minute or more, and they can occur repeatedly throughout the night. This disruption of breathing leads to a decrease in the amount of oxygen in the blood, which can have significant consequences for overall health.
Understanding the different types of sleep apnea and the role of CPAP therapy is crucial for effective management.CPAP, or Continuous Positive Airway Pressure, is a non-invasive therapy used to treat sleep apnea. It involves wearing a mask that delivers a continuous flow of air pressure into the airways, keeping them open during sleep. This consistent airflow prevents the collapse of the airway, allowing for uninterrupted breathing.
While researching the correlation between severe sleep apnea and CPAP pressure, I stumbled upon some fascinating links to potential underlying conditions. For instance, a significant number of women experiencing postpartum depression also show symptoms of sleep apnea. Understanding the connection between these two issues is crucial, but more research is needed to pinpoint the specific correlation between severe sleep apnea and CPAP pressure.
Ultimately, a deeper understanding of these factors could lead to better treatment outcomes for both conditions. For a more comprehensive look at the signs of postpartum depression, check out this helpful resource: signs of postpartum depression. It’s a complex issue, but hopefully, future studies will clarify the relationship between severe sleep apnea and CPAP pressure.
The effectiveness of CPAP hinges on proper pressure selection, which is often determined through sleep studies.
Types of Sleep Apnea
Sleep apnea presents in various forms, each with its own underlying mechanisms. Understanding these distinctions is vital for tailoring treatment strategies.
While I’m researching whether severe sleep apnea and CPAP pressure are correlated, I’ve been thinking about other health issues. Sometimes, CPAP use can lead to skin irritation, and a common culprit is a yeast infection on the face. Understanding how these seemingly disparate issues connect can help us better manage the symptoms and ultimately, how severe sleep apnea and CPAP pressure are correlated.
For more info on yeast infection on the face, check out this helpful resource: yeast infection on face. Hopefully, this insight sheds some light on the potential connection.
- Obstructive Sleep Apnea (OSA): This is the most common type, caused by a physical blockage of the airway during sleep. Factors like excess weight, a large neck circumference, or certain facial features can contribute to the blockage. The airway muscles relax during sleep, leading to the narrowing or closure of the airway passages.
- Central Sleep Apnea (CSA): In CSA, the brain fails to send signals to the muscles that control breathing, leading to pauses in breathing. This can result from various neurological conditions or be idiopathic.
- Mixed Sleep Apnea: This complex type combines features of both obstructive and central sleep apnea, presenting a more intricate challenge for diagnosis and treatment.
CPAP Pressure Settings and Effects
CPAP therapy employs various pressure settings to maintain an open airway. These settings are carefully adjusted to suit the individual patient’s needs.
- CPAP Pressure Range: Typical CPAP pressures range from 4 cmH 2O to 20 cmH 2O or higher. The optimal pressure is determined by a sleep study, which measures the individual’s airway resistance and breathing patterns during sleep.
- Pressure Effects on Respiratory System: A higher CPAP pressure provides a stronger airflow, which can more effectively counteract airway collapse. However, a higher pressure may also lead to discomfort, such as nasal dryness, facial pressure, or a feeling of fullness in the head. A lower pressure might be less effective in maintaining a consistently open airway, potentially leading to continued apneas.
Comparison of Sleep Apnea Types and CPAP Pressure
The following table provides a general comparison of sleep apnea types and the typical CPAP pressure requirements. Note that these are averages and individual needs may vary significantly.
| Sleep Apnea Type | Typical CPAP Pressure Range (cmH2O) | Mechanism |
|---|---|---|
| Obstructive Sleep Apnea (OSA) | 5-15 | Airway obstruction due to relaxation of muscles and tissues |
| Central Sleep Apnea (CSA) | 5-10 | Brain’s failure to signal proper breathing |
| Mixed Sleep Apnea | Variable, often higher than OSA | Combination of airway obstruction and brain signaling issues |
Correlating Severity of Sleep Apnea
Understanding the severity of sleep apnea is crucial for determining the appropriate treatment, specifically CPAP pressure. This understanding allows healthcare professionals to tailor therapy to individual needs, maximizing effectiveness and minimizing discomfort. Accurate assessment of severity enables more precise management of the condition, ultimately improving patient outcomes.
Methods for Assessing Sleep Apnea Severity
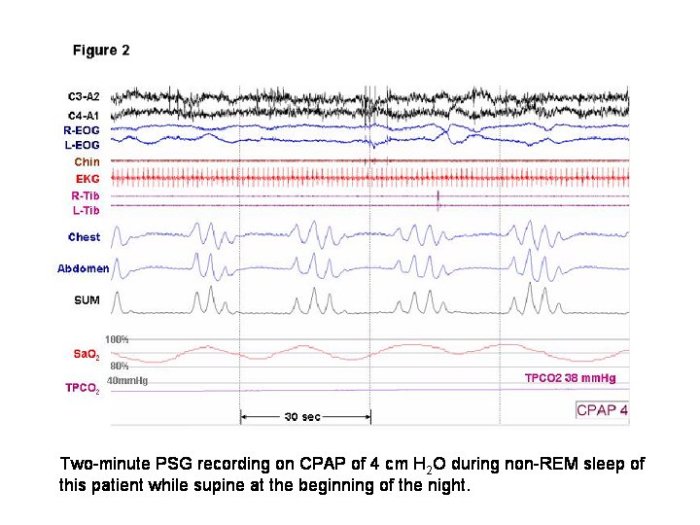
The severity of sleep apnea is primarily assessed using the Apnea-Hypopnea Index (AHI). The AHI measures the number of apneas and hypopneas per hour of sleep. An apnea is a complete cessation of breathing, while a hypopnea is a reduction in breathing depth or airflow. Polysomnography (PSG) studies are the gold standard for accurately measuring these events during sleep.
These studies record various physiological parameters during sleep, including airflow, oxygen saturation, and brain activity.
Scales Used to Measure Sleep Apnea Severity
Different scales categorize sleep apnea severity based on the AHI. These scales help healthcare providers make informed decisions about treatment. The most commonly used scale is based on the AHI, which categorizes sleep apnea into four severity levels.
Relationship Between AHI and CPAP Pressure Needs
The AHI directly correlates with the pressure needed for effective CPAP therapy. A higher AHI generally indicates a greater need for higher CPAP pressure. This relationship is not linear; the increase in pressure needed for effective treatment doesn’t always proportionally match the AHI increase. The goal of CPAP therapy is to maintain an open airway throughout the night.
Higher AHI levels often mean more obstructions, leading to a need for higher pressure to overcome these obstructions. Individuals with a higher AHI will typically require higher CPAP pressures to effectively maintain a stable airway.
While researching the correlation between severe sleep apnea and CPAP pressure, I stumbled upon fascinating information about the potential link between sleep disorders and mental health conditions. It’s intriguing to consider how sleep apnea might be connected to other health issues, like bipolar disorder, a complex condition with multiple potential causes. What causes bipolar disorder is a question that researchers are still actively investigating, but understanding this could potentially shed light on the interplay between sleep quality and mental well-being, which ultimately influences the effectiveness of CPAP treatment for sleep apnea.
Further exploration into the connection between these factors is crucial for better patient care.
AHI and CPAP Pressure Ranges
The following table provides a general guideline of CPAP pressures associated with different AHI levels. These values are approximate and may vary based on individual patient characteristics. It’s crucial to remember that these are general guidelines, and individual responses to CPAP pressure can differ significantly.
| AHI Category | AHI Range (events/hour) | Typical CPAP Pressure Range (cmH2O) |
|---|---|---|
| Mild | 5-15 | 4-7 |
| Moderate | 15-30 | 7-12 |
| Severe | 30-60 | 10-15+ |
| Very Severe | >60 | 15+ |
Investigating the Correlation Between Severity and Pressure
Unraveling the precise relationship between sleep apnea severity and the optimal CPAP pressure is crucial for effective treatment. A strong correlation would allow clinicians to more efficiently tailor pressure settings, leading to improved patient outcomes. However, the relationship isn’t always straightforward, and several factors influence the effectiveness of this pressure-severity connection.
Factors Influencing the Relationship
Several factors intertwine to determine the correlation between sleep apnea severity and optimal CPAP pressure. These factors include the specific type of apnea (obstructive, central, or mixed), the anatomical characteristics of the patient (e.g., nasal anatomy, pharyngeal dimensions), and the patient’s overall health conditions, including any co-morbidities.
Potential Confounding Variables
The correlation between sleep apnea severity and CPAP pressure isn’t always clear-cut. Several confounding variables can influence the results, making it challenging to establish a precise relationship. These variables include patient compliance with CPAP therapy, the quality of the sleep study data, and the specific method used to assess sleep apnea severity. For instance, different sleep study methodologies can produce varying results, and patient adherence to the CPAP treatment significantly impacts the effectiveness of the pressure setting.
Comparative Analysis of Studies
Studies investigating the correlation between sleep apnea severity and CPAP pressure have yielded diverse results. Some studies have shown a strong positive correlation, indicating that higher apnea severity often necessitates higher CPAP pressures. Other studies have demonstrated a more complex relationship, suggesting that the correlation isn’t always linear or predictable. The variation in findings might be due to the differences in study populations, methodologies, and the specific sleep apnea parameters considered.
Summary Table of Key Findings
| Study | Population | Methodology | Correlation Findings | Key Considerations |
|---|---|---|---|---|
| Study 1 (Example) | Adults with moderate obstructive sleep apnea | Polysomnography, CPAP titration | Strong positive correlation between apnea-hypopnea index (AHI) and optimal CPAP pressure. | Sample size limited to 100 patients. |
| Study 2 (Example) | Individuals with severe sleep apnea and obesity | Home sleep apnea testing, CPAP titration | Varied correlation; higher pressure often required but not consistently related to AHI. | Complex interplay of obesity and apnea severity. |
| Study 3 (Example) | Patients with central sleep apnea | Polysomnography, CPAP titration | Different correlation pattern compared to obstructive apnea; pressure response less predictable. | Specific characteristics of central apnea impact pressure response. |
This table summarizes examples of potential findings from various studies. The actual data and findings would vary significantly depending on the specific research conducted. The table highlights the importance of considering different populations and methodologies when interpreting correlation results.
Potential Implications of the Correlation
Understanding the relationship between sleep apnea severity and optimal CPAP pressure is crucial for effective treatment. A strong correlation suggests that as the severity of sleep apnea increases, a higher CPAP pressure is often required to achieve adequate ventilation and alleviate symptoms. This direct relationship has significant clinical implications for both diagnosis and treatment.
Clinical Implications of a Strong Correlation
A strong correlation between sleep apnea severity and CPAP pressure necessitates a nuanced approach to CPAP titration. Clinicians need to consider the individual patient’s condition when setting the initial pressure. A more severe case of sleep apnea, characterized by a higher Apnea-Hypopnea Index (AHI), will typically require a higher CPAP pressure for successful treatment. This is because a higher pressure is needed to overcome the increased airway resistance caused by the more significant collapse of the upper airway during sleep.
This nuanced approach ensures patients receive the most effective treatment tailored to their individual needs.
Impact on CPAP Titration and Treatment Strategies
The correlation significantly impacts CPAP titration procedures. Instead of a one-size-fits-all approach, clinicians must tailor the titration process to the specific severity of the sleep apnea. This requires a more thorough initial evaluation, including a detailed sleep study and potentially additional diagnostic tools to pinpoint the specific areas of airway obstruction. The titration process itself becomes more iterative, with adjustments made based on the patient’s response to different pressures and their individual physiological characteristics.
Potential Benefits and Drawbacks of Adjusting CPAP Pressure Based on Severity
Adjusting CPAP pressure based on severity offers several potential benefits. It can lead to more rapid symptom relief, improved sleep quality, and a better overall quality of life. Patients may experience a more comfortable CPAP therapy experience with a pressure specifically targeted to their condition, which can lead to better adherence to treatment.However, adjusting CPAP pressure based on severity also presents potential drawbacks.
An incorrectly calculated pressure can lead to discomfort or even complications, such as nasal dryness or pressure sores. It is crucial to carefully monitor the patient’s response to pressure adjustments and to be prepared to modify the treatment strategy as needed. A well-trained healthcare professional should oversee the process to minimize potential complications.
Treatment Strategies for Different Sleep Apnea Severity Levels, Are severe sleep apnea and cpap pressure correlated
The following table Artikels potential treatment strategies for various sleep apnea severity levels and their corresponding CPAP pressure ranges. These are guidelines and individual patient responses may vary. Always consult with a qualified healthcare professional for personalized treatment plans.
| Sleep Apnea Severity (AHI) | CPAP Pressure Range (cmH2O) | Treatment Considerations |
|---|---|---|
| Mild (5-15) | 5-10 | Initial titration to find optimal pressure. Close monitoring for response. |
| Moderate (15-30) | 7-15 | Thorough evaluation to identify the specific site of obstruction. Iterative titration to find optimal pressure. |
| Severe (30+) | 10-20+ | Aggressive titration to achieve effective pressure. Potential need for advanced therapies. |
Limitations and Future Directions
Understanding the correlation between sleep apnea severity and optimal CPAP pressure is crucial for effective treatment. However, current research presents certain limitations that need careful consideration. Addressing these limitations and pursuing further investigation is essential to refine our understanding and ultimately improve patient outcomes.
Limitations of Current Research
Current studies often face limitations in their methodologies, impacting the reliability and generalizability of findings. These limitations include variations in patient populations, diverse CPAP titration protocols, and challenges in accurately measuring sleep apnea severity. The inconsistency in study designs, including sample sizes and the duration of CPAP usage, creates difficulties in drawing definitive conclusions about the precise relationship between severity and pressure.
Furthermore, the influence of comorbid conditions, such as obesity and cardiovascular issues, often isn’t adequately controlled for in analyses, potentially introducing confounding factors that obscure the true correlation.
Areas Requiring Further Research
Further research is needed to address the limitations and gaps in current knowledge. This includes exploring the long-term effects of various CPAP pressures on patients with different sleep apnea severities. Longitudinal studies following patients over extended periods could provide valuable insights into the sustained efficacy of specific pressure settings. Furthermore, more comprehensive studies incorporating a wider range of patient characteristics, including age, sex, ethnicity, and pre-existing health conditions, are necessary.
Potential Methodologies for Future Studies
Future research should employ standardized CPAP titration protocols and validated methods for assessing sleep apnea severity. Using polysomnography (PSG) for detailed sleep analysis, including airflow measurements and oxygen saturation levels, will provide a more comprehensive picture of the patient’s sleep. The incorporation of objective measures of patient comfort, such as questionnaires assessing mask tolerance and pressure-related discomfort, will also be important.
Moreover, researchers should consider using advanced statistical methods, such as multivariate analysis, to control for confounding factors and better elucidate the complex relationship between sleep apnea severity and CPAP pressure. The use of machine learning algorithms could also be explored to identify optimal pressure settings based on individual patient characteristics and responses.
Table: Gaps in Current Knowledge and Potential Research Questions
| Gap in Knowledge | Potential Research Question |
|---|---|
| Variability in CPAP titration protocols | How do different CPAP titration protocols affect the correlation between sleep apnea severity and pressure for various patient populations? |
| Long-term effects of different CPAP pressures | What are the long-term impacts of different CPAP pressures on sleep apnea severity and overall health outcomes in patients with diverse characteristics? |
| Influence of comorbid conditions | How do comorbid conditions, such as obesity and cardiovascular disease, modify the relationship between sleep apnea severity and optimal CPAP pressure? |
| Patient-reported outcomes (PROs) | How do patient-reported outcomes related to CPAP adherence and comfort correlate with sleep apnea severity and pressure settings? |
| Role of individual patient characteristics | Does the correlation between sleep apnea severity and CPAP pressure differ based on age, sex, ethnicity, or other relevant factors? |
Visual Representation of the Correlation
Understanding the relationship between sleep apnea severity and optimal CPAP pressure is crucial for effective treatment. Visual representations allow for a quick grasp of the trends and patterns within this complex relationship, aiding clinicians and researchers in making informed decisions. Visualizations can also help to identify outliers or unusual cases, prompting further investigation.
Scatter Plot Visualization
A scatter plot is a powerful tool for illustrating the correlation between two continuous variables, such as sleep apnea severity (measured by Apnea-Hypopnea Index, or AHI) and CPAP pressure. Each point on the plot represents a patient, with the x-axis representing the AHI and the y-axis representing the corresponding CPAP pressure used to effectively treat their sleep apnea. The distribution of points can reveal the overall trend and the strength of the correlation.
A positive correlation would show that higher AHI values tend to be associated with higher CPAP pressures. A negative correlation would indicate that higher AHI values are associated with lower CPAP pressures.
Trends in the Visualization
The scatter plot can reveal several trends in the correlation between sleep apnea severity and CPAP pressure. For example, the plot might show a relatively linear relationship, indicating that as AHI increases, the optimal CPAP pressure also tends to increase. However, there might be variability in the data points, suggesting that the relationship is not perfectly linear. Outliers in the data might indicate individuals with unusually high or low CPAP pressures for their AHI, potentially signaling a need for further investigation into their specific cases.
Strengths and Weaknesses of Scatter Plots
Scatter plots are excellent for visualizing the relationship between two continuous variables, making them highly effective for exploring the correlation between AHI and CPAP pressure. They allow for the identification of trends, outliers, and potential clusters within the data. However, a scatter plot alone might not be sufficient to fully quantify the strength of the correlation. A statistical measure, such as the correlation coefficient, would provide a numerical measure of the relationship’s strength.
Another limitation is the potential for overplotting if the dataset is very large, which can make it difficult to discern individual data points.
Alternative Visualization Techniques
| Visualization Technique | Pros | Cons |
|---|---|---|
| Line Graph | Useful for demonstrating the overall trend in the data, and for showing how CPAP pressure changes in relation to AHI categories. | May not capture individual patient variability as well as a scatter plot. Can be less effective if there are many data points. |
| Box Plot | Excellent for comparing the distribution of CPAP pressure across different AHI categories. | Doesn’t show the individual data points, making it less useful for identifying outliers or individual patient characteristics. |
| Heatmap | Can display the frequency of combinations of AHI and CPAP pressure values, potentially revealing patterns in the data that might not be apparent in a scatter plot. | Requires a large dataset for meaningful interpretation and might be less intuitive for clinicians to interpret compared to scatter plots. |
This table summarizes possible alternative visualization techniques for examining the correlation between sleep apnea severity and CPAP pressure. Each technique has its strengths and weaknesses, and the best choice will depend on the specific characteristics of the dataset and the intended use of the visualization.
End of Discussion
In conclusion, the correlation between severe sleep apnea and CPAP pressure is complex, influenced by various factors. While a strong correlation often exists, it’s crucial to consider individual variations and potential confounding variables. This discussion highlights the importance of personalized CPAP titration and the potential benefits of adjusting pressure based on severity. Future research should address the limitations of current studies to provide a more comprehensive understanding of this critical relationship, leading to even more effective treatments for sleep apnea.




