Fibromyalgia CFS and new injuries often intertwine, creating a complex web of pain and challenges for those affected. This exploration delves into the characteristics of fibromyalgia (FMS) and chronic fatigue syndrome (CFS), examining their overlap and distinctions. We’ll also discuss how new injuries can exacerbate existing symptoms, and the potential long-term implications. The journey through treatment approaches, lifestyle adjustments, and the intricate interplay between conditions will be explored, with a focus on pain management strategies.
Finally, we’ll examine the prognosis and future research directions.
Understanding the unique characteristics of FMS and CFS is crucial for effective management. This involves a detailed explanation of the diagnostic criteria, typical symptoms, and the potential impact on daily life. We’ll compare and contrast the current research and understanding of these conditions, providing a comprehensive overview of their individual and combined effects. Tables summarizing key differences, injury impact, and treatment options will aid in visualization and comprehension.
Understanding Fibromyalgia and CFS: Fibromyalgia Cfs And New Injuries
Navigating the complexities of chronic pain conditions like fibromyalgia (FMS) and chronic fatigue syndrome (CFS) can be challenging. Both conditions present significant hurdles for those affected, impacting daily life and often leading to misunderstandings. This exploration delves into the characteristics, symptoms, overlaps, and distinctions between these conditions, offering a clearer understanding of their impact.
Characteristics of Fibromyalgia Syndrome (FMS)
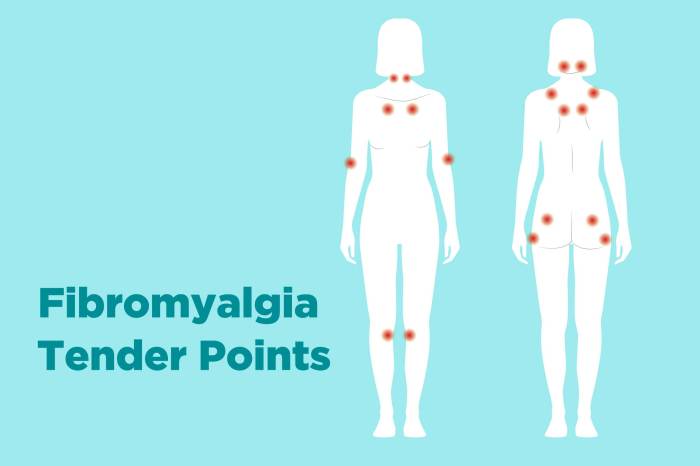
Fibromyalgia syndrome is characterized by widespread musculoskeletal pain accompanied by fatigue, sleep disturbances, and cognitive difficulties. The pain is often described as a deep, aching pain that can affect multiple areas of the body simultaneously. Patients often experience tenderness in specific points (trigger points) that, when pressed, can reproduce or exacerbate pain elsewhere.
Symptoms Associated with Chronic Fatigue Syndrome (CFS)
Chronic fatigue syndrome is primarily defined by profound and persistent fatigue that significantly interferes with daily activities. This fatigue is not alleviated by rest and can be accompanied by a range of other symptoms, including headaches, muscle pain, cognitive impairment (brain fog), and sleep disturbances. A critical factor is the duration and intensity of the symptoms, which often last for months or years.
Overlap and Distinctions Between FMS and CFS
Both fibromyalgia and CFS share overlapping symptoms like fatigue, sleep problems, and cognitive difficulties. However, a key distinction lies in the primary complaint. FMS is primarily characterized by widespread pain, while CFS is primarily defined by overwhelming fatigue. The severity and duration of these symptoms can also vary significantly between individuals.
Diagnostic Criteria for Both Conditions
Diagnosing both conditions relies on a combination of symptom evaluation and exclusion of other potential causes. No single test definitively diagnoses either condition. The diagnostic criteria for FMS typically involve widespread pain in multiple areas of the body and tenderness at specific points. CFS diagnostic criteria usually involve persistent fatigue lasting for at least six months, coupled with other symptoms like muscle pain and cognitive impairment.
Current Research and Understanding
Current research continues to explore the underlying mechanisms of both conditions. While the exact causes remain unclear, research suggests potential roles for genetic predisposition, environmental factors, and the interplay of the nervous system and immune system. Scientists are investigating potential biomarkers and developing more refined diagnostic tools.
Potential Impact on Daily Life
Both conditions can significantly impact daily life. The persistent pain and fatigue can limit physical activity, social interactions, and participation in work or school. This can lead to social isolation, financial strain, and emotional distress. Individuals with these conditions may require significant support systems and accommodations to manage their symptoms.
Key Differences Between FMS and CFS
| Feature | Fibromyalgia Syndrome (FMS) | Chronic Fatigue Syndrome (CFS) | Distinguishing Factors |
|---|---|---|---|
| Primary Complaint | Widespread musculoskeletal pain | Profound and persistent fatigue | Pain vs. Fatigue |
| Typical Symptoms | Widespread pain, tenderness at trigger points, sleep disturbances, cognitive difficulties | Extreme fatigue, headaches, muscle pain, cognitive impairment, sleep disturbances | Pain is a significant feature in FMS, while fatigue dominates CFS. |
| Diagnostic Criteria | Widespread pain in multiple areas, tenderness at specific points | Persistent fatigue lasting at least six months, plus other symptoms | Criteria focus on the nature of symptoms and duration. |
| Underlying Mechanisms | Potential roles for genetics, environment, and nervous system/immune system interplay | Potential roles for genetics, environment, and nervous system/immune system interplay | Research is ongoing for both conditions. |
Impact of New Injuries
New injuries can have a devastating impact on individuals already living with fibromyalgia (FMS) and chronic fatigue syndrome (CFS). The complex interplay of existing pain and fatigue with the added trauma of a new injury can create a vicious cycle of worsening symptoms and reduced quality of life. Understanding these effects is crucial for effective management and support.The presence of FMS and CFS significantly alters how the body responds to injury.
The already heightened sensitivity to pain and fatigue in these conditions often leads to a more pronounced reaction to new trauma. This can manifest as an increase in pain beyond what might be expected in a healthy individual, and prolonged recovery times. The psychological toll can be just as profound, contributing to feelings of frustration, helplessness, and decreased self-efficacy.
Mechanisms of Exacerbation
The body’s natural inflammatory response to injury is often amplified in individuals with FMS and CFS. This heightened inflammatory response can lead to increased pain and fatigue, making recovery from the injury more challenging. Furthermore, the central nervous system’s processing of pain signals may be altered, leading to a misinterpretation of pain signals and a greater perception of discomfort.
The already existing fatigue and sleep disturbances can further impede the body’s ability to heal and recover.
Physical Effects of New Injuries
New injuries can severely impact the physical functioning of individuals with FMS and CFS. The pain and fatigue associated with these conditions often limit movement and participation in daily activities. A new injury can significantly reduce the range of motion and ability to perform tasks, potentially leading to increased dependence on others. Muscle weakness and atrophy can occur due to decreased activity and the persistent pain.
Dealing with fibromyalgia, CFS, and new injuries can be incredibly challenging. It’s a constant juggling act of managing pain and figuring out what’s causing flare-ups. Sometimes, seemingly minor things can trigger a cascade of symptoms. For example, you might wonder if a recent illness, like a potential case of mono, could be contributing to your current issues.
Knowing if you can get mono twice is a crucial piece of the puzzle when assessing the impact of past illnesses on your current health journey. If you’re curious about the possibility of re-infection, checking out this resource on can you get mono twice might offer some insights. Ultimately, it’s essential to connect with healthcare professionals to pinpoint the exact causes and develop a tailored treatment plan for your fibromyalgia, CFS, and new injuries.
Furthermore, the impact of the injury can lead to secondary complications such as joint stiffness, muscle spasms, and reduced mobility. For instance, a sprained ankle in an individual with FMS could result in prolonged immobilization, leading to muscle weakness and difficulty walking, impacting their ability to perform everyday tasks.
Psychological Effects of New Injuries
The psychological impact of a new injury on individuals with FMS and CFS is substantial. The experience of chronic pain and fatigue can create feelings of anxiety, depression, and isolation. A new injury can exacerbate these feelings, leading to a sense of hopelessness and a decline in mental well-being. The inability to participate in desired activities and the fear of further injury can also contribute to feelings of frustration and helplessness.
The individual might experience a decreased sense of self-efficacy and control over their life, further impacting their mental health.
Common Types of Injuries
Injuries commonly affecting individuals with FMS and CFS include:
- Sprains and strains: These injuries, often stemming from overuse or sudden movements, can significantly impact mobility and pain tolerance. A common example is a sprained ankle, which can cause severe pain and limit walking ability in someone with FMS.
- Soft tissue injuries: These can include muscle tears, bruises, and whiplash, often occurring from falls or accidents. The pain and swelling associated with these injuries can be particularly debilitating for those with FMS and CFS.
- Joint injuries: Conditions like osteoarthritis or rheumatoid arthritis can worsen existing symptoms. The chronic inflammation and pain associated with these conditions can have a significant impact on daily functioning for those with FMS and CFS.
Impact on Pain Tolerance and Function
The presence of FMS and CFS significantly impacts an individual’s pain tolerance and functional capacity. A new injury can drastically reduce their pain threshold, making even minor movements painful. This can lead to reduced participation in daily activities and social interactions. The impact on function can be extensive, affecting everything from self-care to work and leisure activities.
For example, a simple fall that would result in a minor bruise in a healthy person could cause significant pain and disability in someone with FMS and CFS, potentially leading to a prolonged period of immobility and reduced ability to perform basic tasks.
Severity of Injury Impact
| Injury Type | Pain | Fatigue | Sleep |
|---|---|---|---|
| Sprained Ankle | High | Moderate | Moderate |
| Muscle Strain | Moderate to High | High | High |
| Whiplash | High | High | Very High |
| Fracture | Very High | Very High | Very High |
Note: Severity is rated on a scale of low to very high. The impact can vary greatly depending on the individual and the specific injury.
Treatment Approaches and Management
Navigating the complexities of fibromyalgia (FMS) and chronic fatigue syndrome (CFS), alongside new injuries, demands a multifaceted approach. Effective management hinges on a combination of medical interventions, therapies, and lifestyle adjustments. Individualized plans are crucial, as the impact of these conditions varies significantly from person to person. Understanding the interplay between these factors is essential for developing a personalized treatment strategy.Effective management of FMS, CFS, and new injuries requires a collaborative approach involving healthcare professionals, patients, and caregivers.
Dealing with fibromyalgia, CFS, and new injuries can be tough, especially when you’re trying to manage other health conditions. For example, if you’re taking asthma medication, be sure to research potential side effects, like those found on sites dedicated to asthma medication side effects. Understanding these can help you anticipate potential issues and work with your doctor to find the best approach for managing all your health concerns, including the ongoing challenges of fibromyalgia, CFS, and any new injuries.
The aim is not just to alleviate symptoms but to improve overall well-being and quality of life. This includes strategies for pain management, addressing emotional well-being, and fostering a supportive environment.
Medication and Therapies
Various medications can help manage pain, fatigue, and other symptoms associated with FMS and CFS. These include antidepressants, anti-inflammatory drugs, and pain relievers. Physical therapy, occupational therapy, and counseling are also important components of treatment. They focus on improving mobility, managing daily activities, and addressing the emotional and psychological aspects of these conditions. These therapies can help patients regain functional independence and improve their quality of life.
Pain Management Strategies, Fibromyalgia cfs and new injuries
Pain management is paramount for individuals with FMS, CFS, and new injuries. Strategies range from medication to non-pharmacological approaches like heat therapy, cold therapy, massage, and relaxation techniques. Understanding the interplay of pain and fatigue is essential. Techniques that address both simultaneously are often most effective.
Lifestyle Adjustments
Lifestyle modifications play a crucial role in symptom management. A balanced diet, regular exercise (as tolerated), adequate sleep, stress reduction techniques, and a supportive social network are all essential elements. Consistency and patience are key to seeing improvements.
Rehabilitation After Injuries
Rehabilitation programs after injuries need to be tailored for individuals with FMS and CFS. This requires careful consideration of the individual’s physical limitations and the potential impact of fatigue and pain on their recovery process. Gradual progression, frequent rest periods, and modifications to accommodate symptom fluctuations are vital.
Support Groups and Resources
Access to support groups and resources is critical. These provide a platform for sharing experiences, gaining encouragement, and learning coping mechanisms from others facing similar challenges. Online forums and local support groups can offer valuable assistance.
Dealing with fibromyalgia, CFS, and new injuries can make getting a good night’s sleep incredibly challenging. Finding ways to improve sleep is crucial for managing these conditions, and a sleep cycle iPhone app like sleep cycle iphone app might offer some helpful insights. Tracking sleep patterns and identifying potential sleep disruptions can be really beneficial for pain management and overall well-being, ultimately supporting my recovery journey from these ongoing issues.
Treatment Options Table
| Treatment Option | Pros | Cons | Considerations |
|---|---|---|---|
| Medication (e.g., antidepressants, NSAIDs) | Can alleviate pain and fatigue, potentially improve sleep | Potential side effects, may not be effective for all individuals, may require careful monitoring | Individualized dosage and selection are essential, consult with a physician. |
| Physical Therapy | Improves mobility, strength, and flexibility, addresses specific movement patterns | Can be physically demanding, requires consistency and patience | Tailored programs for FMS and CFS are crucial to accommodate fatigue and pain. |
| Occupational Therapy | Helps adapt daily tasks to accommodate limitations, improves independence | Requires effort and time commitment, may not fully resolve underlying issues | Focus on assistive devices and modifications to the environment is essential. |
| Counseling/Therapy | Addresses emotional and psychological aspects of the condition, improves coping mechanisms | May not be effective for all individuals, may require multiple sessions | Can provide strategies for stress management and emotional regulation. |
Lifestyle Modifications for Improved Well-being
Implementing these lifestyle adjustments can significantly improve well-being for those with FMS, CFS, and new injuries:
- Balanced Diet: A balanced diet rich in fruits, vegetables, and whole grains provides essential nutrients and supports overall health.
- Regular Exercise (as tolerated): Engaging in regular physical activity, even in small amounts, can improve energy levels and mood, but it is essential to listen to the body’s signals and adjust the intensity accordingly.
- Adequate Sleep: Prioritizing sleep hygiene and creating a relaxing bedtime routine is crucial for overall recovery and well-being.
- Stress Reduction Techniques: Incorporating relaxation techniques such as meditation, deep breathing, or yoga can help manage stress and improve overall well-being.
- Supportive Social Network: Maintaining strong social connections can provide emotional support and reduce feelings of isolation.
The Interplay of Conditions
The journey of managing fibromyalgia (FMS) and chronic fatigue syndrome (CFS), especially when coupled with new injuries, is often fraught with complexities. These conditions don’t exist in isolation; they interact in intricate ways, influencing pain perception, treatment response, and overall well-being. Understanding this interplay is crucial for effective management and improved quality of life.The interplay between FMS/CFS and new injuries is characterized by a complex feedback loop.
Pre-existing conditions like FMS/CFS can significantly alter how the body perceives and responds to new injuries. This often leads to a more intense and prolonged pain experience, which can exacerbate existing symptoms and create a vicious cycle.
The Impact on Pain Perception
Pain perception in individuals with FMS/CFS is already heightened. New injuries, no matter how seemingly minor, can trigger a disproportionate pain response, often exceeding the typical experience for someone without these pre-existing conditions. This amplified pain experience is not merely a matter of the injury itself; it’s a result of the body’s altered central nervous system processing. This increased sensitivity can make even routine activities painful and debilitating.
How the Combination Leads to Chronic Pain
The combination of FMS/CFS and new injuries creates a potent recipe for chronic pain. The existing hypersensitivity to pain, coupled with the new injury’s inflammatory response, creates a vicious cycle. The body’s attempt to heal the injury can be interpreted by the central nervous system as further pain signals, perpetuating the cycle of pain and inflammation. This can lead to long-term pain conditions that are challenging to manage.
Treatment Response
The body’s response to treatment for FMS/CFS and new injuries can be markedly different when these conditions coexist. Treatments that are effective for one condition may not be as effective or may even worsen the other. For example, physical therapy designed to strengthen muscles and improve range of motion in a new injury could inadvertently exacerbate FMS/CFS symptoms if not carefully tailored.
Medication responses can also be unpredictable, necessitating careful monitoring and adjustments.
Masking Symptoms
Symptoms of FMS/CFS and new injuries can sometimes mask each other. A person might attribute persistent fatigue to their FMS/CFS, overlooking the potential contribution of a new injury. Similarly, sharp, localized pain from a new injury could be misinterpreted as a typical FMS/CFS flare-up, delaying appropriate treatment for the injury.
Challenges in Diagnosis
Diagnosing the interplay between FMS/CFS and new injuries can be particularly challenging. Symptoms often overlap, making it difficult to isolate the specific contribution of each condition. A comprehensive evaluation, including a detailed medical history, physical examination, and potentially diagnostic imaging, is often necessary to differentiate and understand the intricate interplay.
Potential Progression of Symptoms
The following flowchart Artikels a potential progression of symptoms in individuals with FMS/CFS experiencing new injuries. Note that this is not a universal experience and individual trajectories can vary greatly.
| Stage | Description |
|---|---|
| Stage 1 | Initial injury. Pain is localized and relatively manageable, but may be disproportionately intense due to pre-existing FMS/CFS sensitivity. |
| Stage 2 | Symptoms of the injury become more widespread, and pain intensifies. Fatigue and other FMS/CFS symptoms become more prominent. A cyclical pattern of pain and fatigue emerges. |
| Stage 3 | Chronic pain becomes persistent. Sleep disturbances worsen, and daily functioning is significantly impaired. Treatment becomes less effective, and the patient may experience frustration and despair. |
| Stage 4 | Severe chronic pain, significant disability, and profound impact on overall quality of life. Depression and anxiety may develop. Managing the interplay of conditions becomes a significant and complex challenge. |
Prognosis and Future Research
The long-term prognosis for individuals with fibromyalgia (FMS), chronic fatigue syndrome (CFS), and new injuries is complex and varies significantly. Factors such as the severity of the initial conditions, the nature and extent of the new injuries, and individual responses to treatment all play a crucial role in shaping the trajectory of the disease. While there is no cure for these conditions, ongoing research offers hope for improved management and potentially better outcomes in the future.The current research landscape is focused on understanding the underlying mechanisms of FMS/CFS, exploring potential biomarkers, and developing more effective treatments.
Researchers are actively investigating the complex interplay between these conditions and new injuries, aiming to better predict individual responses and tailor interventions.
Potential Long-Term Prognosis
The long-term prognosis for individuals with FMS/CFS and new injuries is largely dependent on the severity of the pre-existing conditions and the impact of the new injuries. Some individuals may experience significant improvements in their symptoms with appropriate treatment and management strategies, while others may experience persistent symptoms and reduced quality of life. It’s crucial to acknowledge the variability in individual responses to treatment and the impact of lifestyle factors.
Current Research Efforts
Current research efforts are multifaceted, encompassing numerous areas. Studies are exploring potential genetic and environmental factors that contribute to the development of FMS/CFS, investigating the role of the immune system, and examining the impact of neurochemical imbalances. Furthermore, research is focused on identifying biomarkers that could help diagnose and monitor these conditions, leading to earlier and more precise interventions.
For example, investigations into the role of inflammatory markers and gut microbiome composition are gaining significant traction.
Gaps in Current Knowledge and Future Research Directions
Despite significant advancements, substantial gaps remain in our understanding of FMS/CFS. Key areas requiring further investigation include the precise mechanisms linking new injuries to the exacerbation of pre-existing conditions, and the identification of specific treatment targets for different symptom presentations. Furthermore, research is needed to develop more effective diagnostic tools that can accurately distinguish FMS/CFS from other conditions with overlapping symptoms.
Potential Impact of New Research on Treatment Strategies
New research findings have the potential to revolutionize treatment strategies for FMS/CFS and new injuries. For example, if research identifies specific biomarkers associated with symptom flares, this could lead to earlier intervention and more personalized treatment approaches. Furthermore, a better understanding of the neurobiological mechanisms involved could open up new avenues for targeted therapies, potentially reducing the severity and frequency of symptoms.
Examples of Technological Advancements Affecting Future Treatments
Technological advancements such as wearable sensors and advanced imaging techniques are already providing valuable insights into the physiological changes associated with FMS/CFS. For instance, wearable sensors can track subtle changes in movement patterns and pain levels, potentially enabling more objective assessment of symptoms and facilitating personalized treatment plans. Similarly, advancements in brain imaging technologies could reveal subtle changes in brain activity related to pain perception, potentially leading to the development of new therapies.
Key Areas Requiring Further Investigation
- Understanding the role of the central nervous system in the development and maintenance of FMS/CFS symptoms: This includes investigating the specific neurochemical pathways involved and the impact of new injuries on these pathways.
- Developing more precise diagnostic criteria: This is crucial to differentiate FMS/CFS from other conditions with overlapping symptoms and to identify patients who would benefit most from specific interventions.
- Identifying specific biomarkers for FMS/CFS and new injuries: This would facilitate early diagnosis, personalized treatment, and monitoring of disease progression.
- Investigating the impact of lifestyle factors on symptom severity: This includes exploring the relationship between diet, exercise, sleep, and stress management on the course of the conditions.
- Developing non-pharmacological interventions: This involves exploring new and effective non-medication approaches such as targeted therapies, physical rehabilitation programs, and mindfulness techniques.
Epilogue
In conclusion, fibromyalgia, CFS, and new injuries form a complex interplay that significantly impacts an individual’s health and well-being. The multifaceted nature of these conditions necessitates a personalized approach to treatment and management. This exploration has highlighted the importance of comprehensive care, encompassing pain management strategies, lifestyle adjustments, and the potential support of dedicated resources. Future research and technological advancements hold promise for improving diagnosis and treatment, ultimately leading to a better quality of life for those affected.



